August 19, 2013
Welcome to Part 2 of Chapter 22 of Beyond Training: Mastering Endurance, Health & Life, in which you're going continue to discover the two ways your brain breaks, and exactly what you can do about it. If you missed Part 1 you can click here to read it now.
As you learned in the first part of chapter, there are two ways your brain can break: neurotransmitter imbalances and HPA axis dysfunction.
You already learned 8 ways to fix neurotransmitter deficits and imbalances. You're about to learn 4 ways to fix HPA axis dysfunction. If you pay attention to and implement all these fixes, then your brain will be 100% “tuned” – and you'll be prepared for mental and physical performance breakthroughs, not to mention enhanced motivation, decreased distractions and a better mood.
———————————–
What Is HPA Axis Dysfunction?
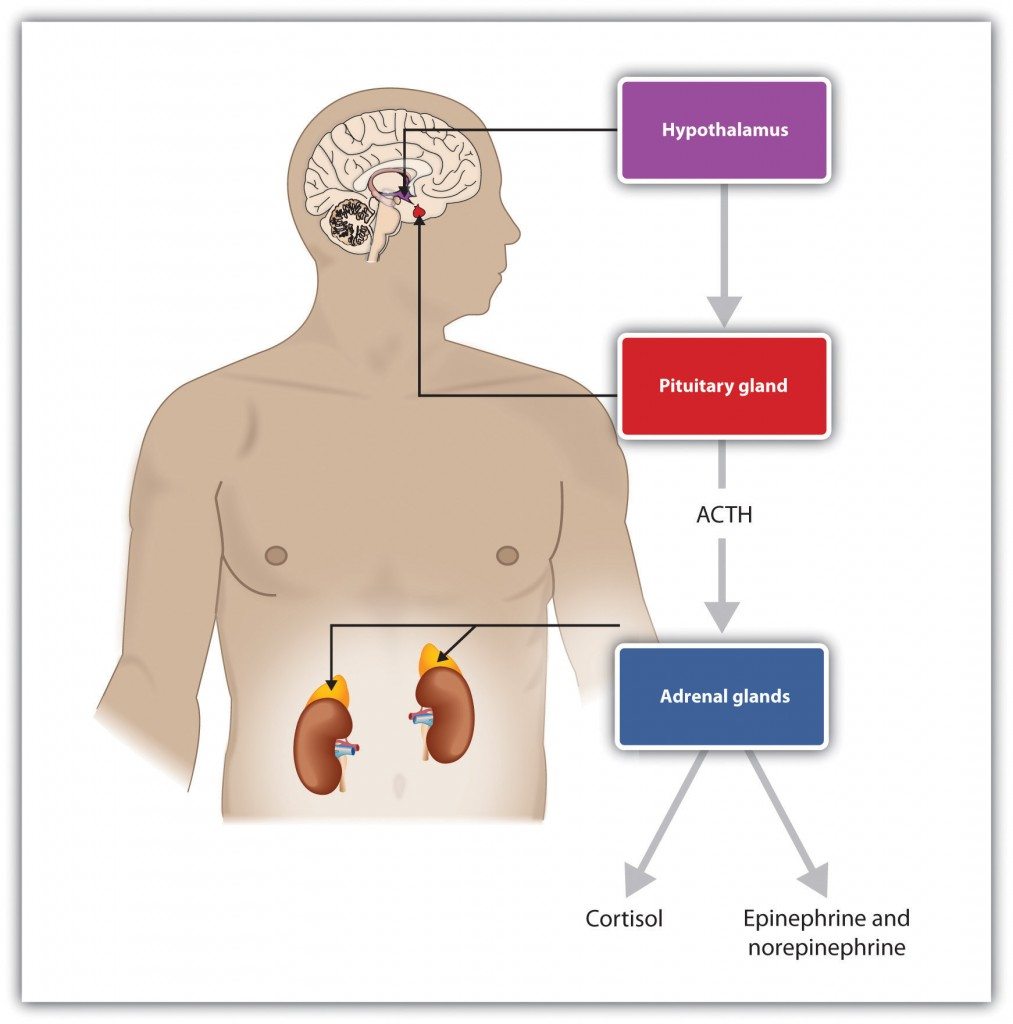
The HPA axis includes three specific parts of your body:
1) the hypothalamus (part of your forebrain);
2) the pituitary gland (just below the hypothalamus);
3) the adrenal glands (at the top of the kidneys).
These three parts work together to regulate functions such as stress response, mood, digestion, immune system, drive, metabolism and energy levels. Before understanding how to fix your HPA axis, it's important to understand how the axis works in the first place, so let's dive into the specific chemicals utilized by your HPA axis.
1. Corticotropin-Releasing Hormone (CRH)
Also referred to as corticotropin-releasing factor (CRF), this hormone is produced and secreted by the hypothalamus in response to stress, and it then stimulates your pituitary gland to secrete adrenocorticotropic hormone. The more stressed your body is (from diet, lifestyle, work, or anything else) the more CRH your hypothalamus will churn out.
2. Adrenocorticotropic Hormone (ACTH)
ACTH is released by the pituitary gland, and travels to your kidneys to stimulate the adrenal glands to increase production of glucocorticoids.
3. Glucocorticoids
The glucocorticoids produced in the adrenal glands are steroids that are necessary regulating metabolic rate, inflammation and immune response. You've already learned about the most notorious glucocorticoids: cortisol.
4. Cortisol
Cortisol is best known for activating our physical response to stress, including injury, lack of sleep, excessive exercise, anxiety, and depression. It prepares your body to withstand these stressful triggers by stimulating norepinephrine (also known as noradrenaline) to active your fight-and-flight reaction.
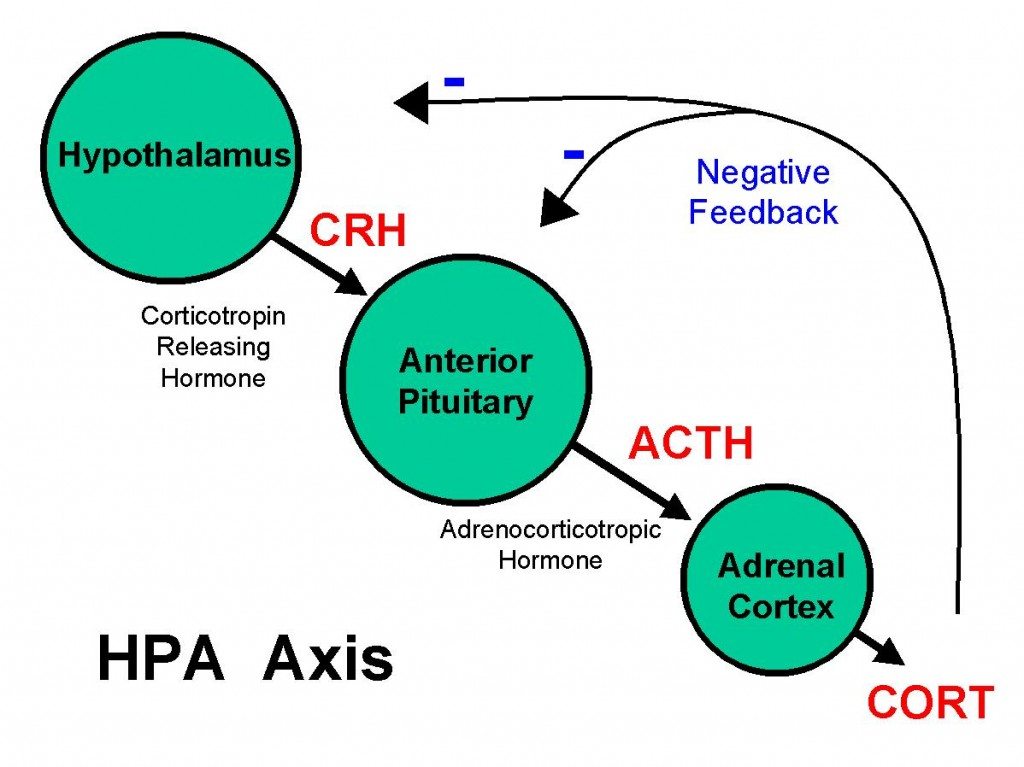
It's important to understand is that your HPA axis operates on feedback loops. A feedback loop occurs when the output of a system in your body somehow loops back to that system as input, and influences its functioning. A positive feedback loop would increase that system's output, and a negative feedback loop would decrease it.
So let's take a look at how a feedback loop would take place in the HPA – in this case with regards to cortisol. At the same time that cortisol activates your fight and flight stress response, it also sends a signal back to your hypothalamus to inhibit CRH production and your pituitary gland to inhibit ACTH. In this feedback loop, cortisol is also able to reduce norepinephrine activity, gradually calming you down and creating a well-functioning checks-and-balances system (3).
In healthy, low-stress individuals this entire HPA axis feedback loop works in harmony. But when cortisol and norepinephrine are chronically overproduced, the HPA axis eventually becomes desensitized to the negative feedback telling it to “calm down”, leading to chronic stress on the hypothalamus, pituitary gland and adrenal glands. Eventually, this leads to the neural failure that eventually causes all the nasty adrenal fatigue issues you learned about in Chapter 6, Chapter 7 and Chapter 8, and it is called HPA axis dysregulation (5).
Interestingly, HPA axis dysregulation is 100% linked to the neurotransmitter imbalance issue you learned about earlier in this chapter. For example, selective serotonin reuptake inhibitor anti-depressants can actually be very effective at treating panic issues. This is because as as serotonin levels rise, levels of norepinephrine fall. Of course, as you also learned earlier, this is not the best way to treat stress, since you'll simply need more and more anti-depressants as time goes on, and your body becomes desensitized to serotonin (2). But it is a good way to point out the fact that as your neurotransmitter production becomes enhanced, you become more equipped to fix HPA axis dysfunction.
Below are 4 additional ways that you can fix HPA axis dysfunction.
———————————————-
4 Ways To Fix HPA Axis Dysfunction
Fortunately, you've already learned in previous chapters just about everything that you need to know about the 4 ways to fix HPA axis dysfunction. Below you will find a quick review. If you address each of these 4 components, your neural feedback loops will be balanced.
I like to think of myself as “stress selfish”. In other words, I guard my brain fairly intensively when it comes to shielding it from stress. I go to bed several minutes earlier than necessary so that when I wake up, I don't need to bolt upright out of bed and rush to my first task. If work gets extremely stressful and I find myself shallow breathing, I go for a walk, or even go lie on the bed, the floor or a couch and do several minutes of deep breathing. I purposefully avoid speaking with people from whom I get “negative energy”. All these little steps add up to protected my HPA axis.
So what else can you do to destress?
Flip back to Chapter 7. There you will see a big list of all the various daily stresses that can disrupt the HPA axis, from scheduling stress to relationship conflicts to poorly designed training equipment or subpar training conditions.
In Chapter 9, (The 7 Best Stress-Fighting Weapons That Will Make Your Mind-Body Connection 100% Bulletproof) you learn that breathing, meditation, tai chi, yoga, coherence, a hobby and high quality sleep are all extremely effective ways to de-stress.
Go back and review those two chapters. Take stress seriously. Do not abuse your body, and your brain will thank you.
———————————–
2. Avoid Excessive Exercise
Overtraining is one of the quickest paths to HPA Axis dysfunction, and leads to many of the brain fog, mood and irritability issues experienced by many athletes, especially endurance athletes.
In my podcast interview with Dr. Sara Gottfried “The Cost Of Being A Bad-Ass – How To Cure Your Hormones With Dr. Sara Gottfried“, Dr. Sara explains how excessive exercise chronically elevates cortisol levels, and tells you what you can do about it. I spell all this out in detail in Chapter 6, Chapter 7 and Chapter 8.
If you've created high cortisol levels from high amounts of exercise, revisit those chapters. Follow the recovery protocols, and also consider supplementation with Chinese Adaptogenic Herbs such as TianChi or InnerPeace, high electrolyte intake, preferably with liquid trace minerals or Himalayan sea salt, 2,000 to 5,000 milligrams of a whole foods Vitamin C source, and 4-6g per day of a good fish oil that preferably contains vitamin E with mixed tocopherols.
Also, as a means of promoting hormone stabilization and hormone balance in a gentle and natural manner -without the use of pharmaceutical or synthetic hormone replacement therapy – try this potent stack. It is comprised of a bottle of trace liquid minerals, a bottle of fish oil, and a box of Chinese Adaptogenic Herbs. If you've been engaged in excessive exercise, this can help bring your HPA axis back into balance.
———————————–
When I wake up with a “fuzzy brain” (which can happen after a late night out, too much alcohol, or getting sleep disrupted during the night), one of the first things I do is pop 1000mg of curcumin from Phenocane, which can rapidly shut down inflammation and mitigate the effect of a poor night's sleep on the HPA axis. This is because curcumin is a potent anti-inflammatory.
Decreasing inflammation is a potent HPA axis protecting and repair strategy. In mice, researchers have experimented with a protein involved in inflammation in the hypothalamus called NF-kB. When NF-kB is switched off in the hypothalamus of the mice, they lived about 20% longer (6). On the flip side, increasing NF-kB not only accelerates aging, but also decreases an important another important brain protein called GnRH. When GnRH is turned down, fewer new brain cells are created, and aging is accelerated even more (1).
This is just one example of how inflammation can affect the HPA axis. Elevated cortisol levels can also cause systemic inflammation (and vice versa), which further aggravates the HPA axis.
As you learned in Chapter 8, maximizing intake of anti-inflammatory foods and minimizing pro-inflammatory foods is just one step toward controlling inflammation, and from fish oil to cold thermogenesis to pulsed electromagnetic field therapy, there are a couple dozen other strategies in that chapter that will decrease inflammation. Most of those anti-inflammatory protocols work not only on the muscles, but also on the HPA axis.
———————————–
In Chapter 7, “The Last Resource You’ll Ever Need To Get Better Sleep, Eliminate Insomnia, Beat Jet Lag and Master The Nap” you learn that the only time your body actually repairs neurons and nerve cells is when you are sleeping – especially during deep sleep stages that occur as your body temperature decreases between 2am and 6am.
So if you're attempting to fix your HPA axis and you're not getting quality sleep, then you're never going to fully recover and repair.
As a matter of fact, because of the crucial role that sleep plays in the health of your nervous system, getting adequate sleep is the single most important strategy you could ever implement for fixing your brain and enhancing your mental function.
Even if you incorporate all of the biohacks you'll learn about in the next chapter, you're never going to experience 100% optimal nerve and brain performance if you aren't sleeping properly – and this is all the more true the evening of any day you're doing hard workouts. In the same way that you need to be selfish with stress, you need to be selfish with sleep.
——————————————
Summary
At this point in your reading, you shouldn't be surprised by the four best strategies to fix your HPA axis: de-stress, avoid excessive exercise, shut down inflammation and sleep (Holtorf). You saw these strategies in the recovery chapter too – and there's a reason for that: the more you break down the body the more fragile your brain becomes.
All four of the fixes you've just learned about are interrelated and codependent, and if you get each of them dialed in, your hypothalamic-pituitary-adrenal feedback loops will work with wonderful efficiency.
In the next chapter, you're going get an amazing array of tools, tricks and tips to tune your mind, hack your brain, boost your IQ, enhance your focus and instantly get into the coveted, effortless zone of peak performance.
In the meantime, leave your questions, comments and feedback below!
——————————————
LINKS TO PREVIOUS CHAPTERS OF “BEYOND TRAINING: MASTERING ENDURANCE, HEALTH & LIFE”
Part 1 – Introduction
-Preface: Are Endurance Sports Unhealthy?
-Chapter 2: A Tale Of Two Triathletes – Can Endurance Exercise Make You Age Faster?
Part 2 – Training
-Chapter 3: Everything You Need To Know About How Heart Rate Zones Work
–Chapter 3: The Two Best Ways To Build Endurance As Fast As Possible (Without Destroying Your Body) – Part 1
–Chapter 3: The Two Best Ways To Build Endurance As Fast As Possible (Without Destroying Your Body) – Part 2
–Chapter 4: Underground Training Tactics For Enhancing Endurance – Part 1
–Chapter 4: Underground Training Tactics For Enhancing Endurance – Part 2
–Chapter 5: The 5 Essential Elements of An Endurance Training Program That Most Athletes Neglect – Part 1: Strength
–Chapter 5: The 5 Essential Elements of An Endurance Training Program That Most Athletes Neglect – Part 2: Power & Speed
–Chapter 5: The 5 Essential Elements of An Endurance Training Program That Most Athletes Neglect – Part 3: Mobility
–Chapter 5: The 5 Essential Elements of An Endurance Training Program That Most Athletes Neglect – Part 4: Balance
Part 3 – Recovery
–Chapter 6: How The Under-Recovery Monster Is Completely Eating Up Your Precious Training Time
–Chapter 7: 25 Ways To Know With Laser-Like Accuracy If Your Body Is Truly Recovered And Ready To Train
–Chapter 8: 26 Top Ways To Recover From Workouts and Injuries with Lightning Speed
-Chapter 9: The 7 Best Stress-Fighting Weapons That Will Make Your Mind-Body Connection 100% Bulletproof
-Chapter 10: The Last Resource You’ll Ever Need To Get Better Sleep, Eliminate Insomnia, Conquer Jet Lag and Master The Nap: Part 1
-Chapter 10: The Last Resource You’ll Ever Need To Get Better Sleep, Eliminate Insomnia, Conquer Jet Lag and Master The Nap: Part 2
Part 4 – Nutrition
-Chapter 12: What A Half-Naked Ironman Kickboxing Superhero Can Teach You About How Many Calories, Carbs, Proteins And Fats You Should Be Eating
-Chapter 13: How Much Carbohydrate, Protein and Fat You Need To Stay Lean, Stay Sexy and Perform Like A Beast.
-Chapter 14: The Zen Of Customizing Your Diet To Your Unique Body And Goals
-Chapter 16: The Real Truth About What To Eat Before, During And After Your Workouts & Races.
-Chapter 17: The 21 Best Kitchen Tools, Grocery Shopping Guides, Cookbooks, Websites and Local Resources To Fuel Your Active Lifestyle.
Part 5 – Lifestyle
-Chapter 18: How To Protect Your Body From The 10 Hidden Killers In Your Home.
-Chapter 19: The Zen Of Getting Uber-Fit Without Neglecting Your Friends, Your Family and Your Career.
-Chapter 20: How To Quit Mowing Your Lawn & 10 More Top Time-Saving & Productivity Tips.
Part 5 – The Brain
-Chapter 21: Two Ways Your Brain Breaks And Exactly What You Can Do About It – Part 1
-Chapter 22: Two Ways Your Brain Breaks And Exactly What You Can Do About It – Part 2
——————————————-
REFERENCES
1. Bernard, D. (1999). Photoperiodic effects on gonadotropin-releasing hormone (gnrh) content and the gnrh-immunoreactive neuronal system of male siberian hamsters. Biology of Reproduction, 60(2), 272-276.
2. Carmine M. Pariante, Institute of Psychiatry, King’s College London Depression, stress and the adrenal axis. The British Society for Neuroendocrinology, 2003.
3. Engelmann M, Landgraf R, Wotjak C (2004). “The hypothalamic-neurohypophysial system regulates the hypothalamic-pituitary-adrenal axis under stress: an old concept revisited.”. Front Neuroendocrinol 25 (3-4): 132–49.
4. Holtorf, K. (2008). Diagnosis and treatment of hypothalamic-pituitary-adrenal (hpa) axis dysfunction in patients with chronic fatigue syndrome (cfs) and fibromyalgia (fm). JOURNAL OF CHRONIC FATIGUE SYNDROME, 14(3), 1-14.
5. MacHale SM, Cavanagh JT, Bennie J, Carroll S, Goodwin GM, Lawrie SM (November 1998). “Diurnal variation of adrenocortical activity in chronic fatigue syndrome”. Neuropsychobiology 38 (4): 213–7
6. O'Neill, J. (1997). Nf-kb: a crucial transcription factor for glial and neuronal cell function. Trends in Neuroscience, 20(6), 252-258.





The trick is in supporting brain to open up and to additionally offer a secure area for conversation at a deeper stage. So lots of our interactions is executed on a totally superficial stage. How are you? I’m fine, how are you? That’s simply being well mannered however would not get to the coronary heart of the matter! Things may be festering inside. But we can not confide in simply anyone. There needs to be a few stage of trust. Just some mind at the subject! anyway thank you for sharing this article
Please forward names of Doctors that treat HPA Axis in Detroit area MI or Collier County Fl.
I’m 24 with bad hpa axis from over exercising for years upon years. Recently my once high cortisol dropped and now I’m in the lower end of burnout. I need help and I’ve been to so many drs who don’t recognize this please help me I’m doing so bad I’m out of work and school.
I recommend scheduling a consult at BenGreenfieldFitness.com/coaching … Then we can take a personalized, deep dive into everything that's going on.
This article is incomplete. It simply fails to address the most important factor – SLEEP. What to do to fix sleep? Simply mentioning that sleep is important is not enough. We have already figured that out. It doesn’t take rocket science.
I agree, sleep, or lack of is at the heart of all my health problems.
I would try collagen powder about 1 before bed or raw honey, or both. These have been the only things that have ever helped me sleep and believe me, I’ve tried everything. If worst comes to worse, 3.5-7.5 mg of Remeron will help as well.
It’s in the next chapter; however, here are a few tips:
1. Avoid alcohol or caffeine after a certain time
2. Avoid sugar
3. Try deep breathing exercises while lying down and listening to ambient music
4. Try taking a warm bath with epsom salts
5. Try taking adaptogenic herbs ( if you have high cortisol, Holy Basil)
6. Try taking 5-HTP ( precursor to seretonin)
All of the above have helped me. I hope you’ve found some relief.
Laura
Ditto Laura. And this is exactly what my Dr. recommended also. May consider adding 500 mg Glycine daily to support serotonin.
Also, high impact training (HITT) is now off the list. According to my doc, it’s the worst form of exercise for those struggling with HPA axis dysfunction.
I am a former endurance athelete/marathon runner..after reading so much research in recent years about the deteriment of prolonged exercise and inflammation, muscle and skeletal breakdown, as well as CardioVascualr strain. I have since converted to doing more calesthenics type body weight cardio at home varying exercises and inserting interval. Prior to that i was an everyday runner locally competitive but really did the same thing every day 8-10 miles at similiar pace. What do you make of all the press that long cardio is inferior to the short HITT type exercises with regards to overall health.
Hi~In my “awake” life I call it~ I have incredible eating habits I’m healthy, I’m 47, I stay away from sugars, carbs generally rotten stuff. Until I’m asleep~doing my own research I’ve come up with a “night eating syndrome” where no matter what time I go to sleep I’m up 2 hours after,then about 2 times a night after that. To raid my fridge of carbs, cookies, generally any kind of crap I would not eat in my “awake” life. As I”m not quite awake but not fully sleeping either. Not awake enough to stop the motion. I have mentioned it to every Dr. they laugh and say lock the fridge , which I find ignorant. I had a child @ 40, I’m a single Mom, and it started around her birth and waking to nurse, I just thought it was to feed my body to prepare it for that, but the years are passing and its still going on, I seem to sleep the best from 3-6am. At night I wake up and go right to the fridge or cabinet, craving, I mean CRAVING carbs or junk, or Sodium. I’m aware, but can’t snap out of it~it’s embarrassing, My neurologist put me on topirimate, to curve my appetite I still wake up, I’ve tried staying up really late, eating really late, wine, diff foods so many things, I”m up like clock work. It HAS TO BE deeper than that. I went to an endocrinologist I mention my HPA axis because this makes sense to me your body has to have an axis. A center gound so to speak, she laughed at me!! And because I eat so much at night I compensate by not eating too much during the day. I have broken sleep, I’m not sure what avenue to take to even but this can’t go on. I’m at my whits end. ~By Nature I’m a very wound person, very high energy, I have a very hard job, so there are stresses. But I stay happy, but this issue is a new hitchhiker I want to drop off and I’m having no luck :(
Check this out: https://bengreenfieldfitness.com/2013/08/how-to-f…
I have more here: https://bengreenfieldfitness.com/unbeatable16/
I am not a doctor and this is not to be taken, interpreted or construed as medical advice. Please talk with a licensed medical professional about this. These are just my own personal thoughts and not a prescription or a diagnosis or any form of health care whatsoever.
If you prefer a more direct, customized approach, I'd be happy to help you via a personal one-on-one consult. Just go to https://bengreenfieldfitness.com/coaching. and then choose a 20 or 60-minute consult, whichever you'd prefer. I can schedule ASAP after you get that. Additionally, if I'm "out of your price range" (yes, yes, I know I can be a spendy guy to access) I have a team of coaches I've personally trained who can help you here: https://greenfieldfitnesssystems.com/product-cate…
That’s why you are staying awake at nite and eating carbs. Because you don’t during the day time.. Your adrenals wake you up, Stressed, wanting you to eat.. If you eat before you go to sleep. Let’s say a small cup of vanilla ice cream.. you will start to sleep all throughout the nite.. You must eat some carbs before bed.. Sip on orange juice with salt.. Many strategies to try. (this is why they say Honey helps you sleep throughout the nite.. it’s sugar.. Keeps the adrenals from being stressed.)
I suspect my Cortisol levels are high and I’m awaiting tests to confirm due to prolonged stress and over exercising and dips in mood/anxiety following the gym but found this article on HPA axis fascinating and the recovery process is working wonders with me. I have a question about Serotonin and use of 5 -HTP. Is there a need to take this if HPA axis is recovering as Serotonin will I assume follow and also does taking 5 HTP actually increase Cortisol levels?
thanks in advance
I have used clobetasol propionate topical solution on my scalp twice a day for 2 weeks now for scalp psoriasis..
Is there something I need to be taking to prevent problems with HPA axis?
I wonder if this HPA axis is the key to what’s been going on with me. I’ve been having these episodes frequently but not constantly where, when I get hungry, I start shaking uncontrollably, I feel pressure in my forehead, and my heart races. It takes eating something, maybe drinking some wine, and deep breathing to calm it down. I will most often experience them in the middle of the night but have them during the day too. I have no idea what causes these episodes and would very much like them to stop. I’ve started taking NAC supplements and that has seemed to help calm them down quite a bit. I’ve also been struggling to lose weight and am carrying more weight in my midsection than ever before. I’m 42 years old and this all started about 2.5 years ago after my youngest was born. Any thoughts?
This definitely sounds like it could be HPA axis dysfunction though it's tough to say without seeing your health and medical history, exercise history and current diet. If you want to go into detail, feel free to book a consult at <a href="https://greenfieldfitnesssystems.com/ben” target=”_blank”>www.greenfieldfitnesssystems.com/ben and choose 20 or 60 minutes and we'll get you scheduled for a Skype consult.
Your website has saved my life…now I understand what has been going on in my brain…I kept telling my therapist…I feel like my brain broke ….after a bad virus last year…and getting off all medications….I am still struggling with horrendous episodes of anxiety/depression….
Would you kindly give me your opinion on Maca Root? I take Femmenessence Macapause to balance my hormones…have been for a year…supposed to balance the HPA axis..but I wonder if it is too stimulating?
I wake up around 3:00 am …heart racing…adrenaline or cortisol peaks all night and all day…am in a state of hyperarousal….anxiety that is beyond horrible… please help me….Thanks much!
Aargh…I would really have to see your full health history to make an educated response. I'm sorry! But I'd be happy to help you via a personal one-on-one consult. Just go to https://bengreenfieldfitness.com/coaching. and then choose a 20 or 60 minute consult, whichever you'd prefer. I can schedule ASAP after you get that.
I am also in this boat and would like to know. After a massive breakdown, my HPA axis is constantly geared to stress mode and that’s all. At the moment I have to be in a sedating SNRI that basically suppresses everything including metabolism. It just feel like a band aid fix. When I come off, within 5 days, of relaxing and avoiding stress and exercise, taking Curcumin twice a day, by day 5 I am back at complete exhaustion to the point where the adrenaline is so high I feel like I’m going to lose my mind and go into psychosis or something. So naturally I just go back on the drug. But I need to find a fix for a really messed up axis. This is no way to live.
You have an overactive amygdala mate. I’ve suffered from exactly the same thing in the past and can relate to your post so much. The amygdala is one step upstream from the hpa-axis and is responsible for deciding the autonomic response from the body. If your sympathetic nervous system (fight or flight) is activated it’s because your amygdala instructed the hpa to do so. I have ptsd which caused mine and your massive breakdown would have had a similar affect on your amygdala as my traumatic event did on mine. The amygdala becomes so traumatised by a particular event (or series of events) is becomes hypersensitive and fires off uncontrollably. So its not actually your hpa thats geared to stress mode as you put it it’s your amygdala which the in turn triggers the hpa. The chronic hpa activation is the effect, the overactive amygdala is the cause. Thats why your spot on about the SNRI being a bandaid fix. As long as the amygdala is overactive the problem by definition can’t go away. The beauty of this is the amygdala is extremely plastic and can be manipulated via neuroplasticity extremely effectively. Mindfulness meditation has been scientifically proven to reduce hyper-reactivity of the amygdala and actually shrink it back down to it’s original size. Proven with fMRI scans and all. As little as six weeks of performing mindfulness meditation for 20 minutes a day has been proven to shrink the amygdala to a degree that you can literally see the difference on brain scans. I could literally talk all day about this topic but trust me when I tell you your problem begins and ends entirely with the amygdala, calm it down and it wont constantly trigger your hpa and you will be 100% cured. You seem like a smart guy I know this will lead you down the path of researching the amygdala yourself and discovering all you need to find your solution. I would also suggest buying a digeridoo and taking up playing. Its sounds very obscure I know but it is the most powerful natural form of vagus nerve stimulation known to man and nothing calms the amygdala faster or more that vagus nerve stimulation. Mindfulness is a close second. God bless you.
Hi there- after years of overtraining I finally “broke”. I got a virus from which I never really recovered. I also obviously have hpa dysfunction (intolerant to exercise/fatigue/strange neurological symptoms etc). I am doing all the protocols you suggest and de stressing/mindfulness/acupuncture/yoga/Pilates/ supplements/good diet/tons of sleep. My question is on the excessive exercise- while I don’t want to overtrain again, I wokld like to get back into endurance racing. Is this a realistic goal or do I need to hang up my hat… Wondering what your experience with others in the same boat has been. I would love to know that I could race again..
I would start here: http://home.trainingpeaks.com/products/trainingpl…
This is such a complicated issue. I’m going to try curcumin to see if that helps bring the inflammation down.
True that Julie!
Hi would you be kindly to see a link to my Sleeping condition and see if I am a good candidate any research or place that might be able to treat me? Here is the link:
https://youtu.be/BomKqeQZwVk
My apology if there some negative emotional reaction in the description of the video.
Thank you
I should begin by clarifying the fact that I am *not* a physician and this is *not* to be interpreted as medical advice. Please talk to a licensed medical professional about all of this! I'd be happy to help you via a personal one-on-one consult. Just go to https://bengreenfieldfitness.com/coaching. and then choose a 20 or 60 minute consult, whichever you'd prefer. I can schedule ASAP after you get that.
Thanks for the article . I found the link when I looked up how to fix Hpa axis. I suffer from severe hormonal migraines about 10 days out of the month and I take triptans to help them which have an effect on serotonin. I definitely have leaky gut and suffer from histamine intolerance and severe insomnia. I can’t take supplements because they give me migraines so I am limited in what I can do. I have had my hormones checked but am now wondering if I should try to get the panel with dopamine, serotonin, Gaba etc. I eat a clean Paleo based diet, watch my stress levels, take progestrone and exercise. Anyways I am going around in circles no idea who could possibly help me. Any advice or direction is much appreciated or if any one out there has experienced the same issues and could help out and share with me I would love to hear from you. Thanks
This is kind of a complex question and would be better if you booked a consult at bengreenfieldfitness.com/coaching. Choose 20 or 60 mins and we'll get you scheduled.
I have adrenal fatigue and recently started taking curcumin and NAC I noticed I'm dead tired now and have come onto the internet for some clues. The only thing I can see if that curcumin can lower cortisol so im wondering if I'm making a bad situation worse.
I am taking adaptagen herbs but the biggest fatigue started after the above 2 new supplements. Any idea??
You'd have to take a crapola of curcumin to lower cortisol. In my opinion, you should go to this blog post and pay attention to the very bottom where I talk about all my recommendations for adrenal fatigue:
https://bengreenfieldfitness.com/2013/06/how-t…
Just a reminder I am not a doctor and you should seek advice from a physician also. You can also schedule a one on one consult with me at greenfieldfitnesssystems.com/ben choose a 20 or 60 min consult and we can go over everything.
Dear Ben Greenfield,
I have a few questions regarding HP-Axis, Leaky Gut, Adrenal Fatigue, and TMS (tension myositis syndrome).
Anyways, about a year and a half ago I went under a lot of stress, both emotionally and physically. A family member passed away and I was training heavily and pushed myself too hard. This lasted like 2 months before I started feeling extremely fatigued I eventually got to the point that I couldn't do any sports without being significantly tired. I did all sorts of testing and everything came back normal. I went through naturopathic/alternative medicine and was diagnosed with "leaky gut" , "adrenal fatigue", and neurotransmitter issues.
I tried to stay on an AF protocol – which included a diet and supplements (enzymes, Adr gland support, hormones, vitamins, take mineral) for a few months but didn't feel any better. After loosing hope I went to a Chinese doctor and he gave me some Chinese herbs (mainly ginseng and licorice root) which have helped immensely, but once Im off the herbs I feel bad again.
I've had a hard time accepting the treatment for AF and leaky gut. I think its all mental, especially after reading John Sarno's books on TMS – im not sure if you're familiar with TMS.
So heres my QUESTION: you said that the HP Axis is responsible for creating the stress/cortisol cycle, so if I can cure the HP Axis through the techniques you suggested: destress, excessive exercise, anti-inflammatory, and lots of sleep – then will the AF and Leaky Gut be cured as well? Even without supplements and a diet? I understand that the gut and brain are connected, and that the neurotransmitters can only be re-balanced if you "heal the gut", but is this necessary? If I healed my HP Axis and Neurotransmitters through stress reduction, mindfulness, positive attitude, and working through my emotions – will my gut heal too?
Im just not in a position (financial and time-wise) that I can follow a strict AF diet – it makes me even more stressed trying to follow the diet, and I haven't had any positive results. I am a generally healthy eater but don't avoid gluten or any other foods (even though lately I've become sensitive to them). So, can leaky gut and AF and Hp-Axis be healed with your mind? Or are diet and supplements necessary?
Thank YOU
Taking care of one will certainly help the other but you really need to come at it from both sides. It's not just a one way street. I would look into something like this to incorporate along with your stress lowering protocol https://greenfieldfitnesssystems.com/product/deto…
I use "Relora" (a proprietary blend made by NOW Foods which can be found on Amazon) to control the fight/flight hormone imbalance and calm my nerves. When my bottle arrived, I took the daily max of 3 immediately and felt like 'me' within 90 minutes. Now I take one capsule 3 times a day. In addition, I also take cayenne pepper, turmeric, high dose of Vitamin C and B12 sublingually.
The HPA axis dysfunction I have is from injuries sustained in a car accident nearly a decade ago, so I have other issues I address with other supplements.
Relora is in this: https://bengreenfieldfitness.com/multi !
Since I use Relora 3 times a day, I would be using your 'PM' vitamin 3 times a day as that ingredient is not in the 'AM' vitamin. :)
Hey Ben great site and amazing information.
I suffer from chronic brainfog 24/7 type of thing. Ive had it for about 4 years. About 2-3 times over this period on nights ive drank heavily I woke up with no brain fog, feeling gernerally more connected to the world, have more energy and just generally feeling better (obviously because the brain fog is gone). Now this feeling last for a couple hours and after that all my symptoms come back. What do you think causes this? I havent been able to find any insights to this anywhere. Thanks!
Ps: I usually only drink once a week in moderation. I havent drank in 3 months while also cutting out all wheat, gluten, dairy, and grains. I feel a bit better about 50% to where I want to be but I cant seem to get overt his hump. I also feel tired all the time which I think goes hand in hand with my brain fog. Im a 20 year old male and all my bloodtest have came back normal. Thanks again!
I would look at your gut. There may be something nasty living down there that is creating the brain fog. Check this out – https://bengreenfieldfitness.com/2014/01/step-…
Hi,
THANK YOU for making all of this info available in a free and easy to understand format! I was scouring the NIH data banks for info on benzodiazepine withdrawal on physical stamina then fortunately ran across this. After years of being precribed benzos for seizure disorder I am tapering off and experiencing sudden labile hypertension, tachycardia/bradycardia and a TOTAL incapacity to do any exercise — not even my usual yoga routine. NIH studies on this are slim at best, but a couple suggestion exercise intolerance is caused by disruption of the HPA system by use of, and withdrawal from, benzos and their effect on neurotransmitters. Are you aware of any other research on this and/or any special protocols (other than you have already listed here) for someone like me (60’s) completely unable to exercise, rising BP fluctuating HR and a caring, but totally baffled, Doctor who is trying to help me? Thanks again for sharing all this info. I really appreciate having access to it as this is proving to be such struggle.
Best,
Mo
Tapering off benzodiazepines is EXTREMELY complex. I’ve walked a few clients through it but it would be a matter of consulting with me to discuss your current diet, how long you were on, how much, what times of days, your current blood/gut results, etc. This is NOT something I feel comfortable doing on a blog comment though! I'd be happy to help you via a personal one-on-one consult. Just go to https://bengreenfieldfitness.com/coaching. and then choose a 20 or 60 minute consult, whichever you'd prefer. I can schedule ASAP after you get that.
Periodic Limb Movement Disorder, PLMD or PLMS and previously known as nocturnal myoclonus, is a separate and different disorder from restless leg. Restless leg is a voluntary movement to an urge to move. PLMD is a involuntary movement while you are asleep and prevents the brain from reaching deep sleep because the brain "wakes" from the involuntary movements. The standard treatment for it is the same as Parkinson's disease–dopamine. I do not know how dopamine fits into the HPA axis though.
Interesting. It may be interesting to experiment with something like Mucuna or L-Dopa as a slightly natural way to increase dopamine…although I'm a fan of a pre-sleep romp for that. ;)
So if you have a sleep disorder, like periodic limb movement disorder, and can't sleep, you can't ever repair your brain and stop the HPA axis from continuing to spiral out of control. What do you do then? If you have any advice or links, I would appreciate it because I am in that boat and it's sinking. Thank you for the article.
Do you mean, restless leg syndrome? If so, take a look at this – http://www.quickanddirtytips.com/health-fitness/m… Hopefully it will help you out!
Hi Brightnshiny,
i know you left this comment several years ago, but i’m on a quest to cure my PLMD and found this comment when searching the Ben Greenfield site. I’m hoping to hear if by now you’ve come up with a more natural/safe cure as i also do not care to take the Parkinsons disease medication.
Ben, you prefer phenocane to straight up Curcumin? You'd have to take a lot of phenocane to get the antiinflammatory effects of curcumin.
The "extras" in Phenocane make it THAT much more effective over all for pain management. Curcumin alone is great purely for its anti-inflammatory properties.