September 17, 2019
Not that I'm ever known to do this, but I recently did something quite biomechanically stupid.
A couple Saturdays ago, I raced a triathlon. I raced hard. I won the triathlon, actually. But despite keeping myself in relatively good shape, I haven't been doing much hardcore swim-bike-run training lately and my hips and low back were tight as kevlar cables the next morning.
Nonetheless, I sucked down a stiff cup of coffee and meandered with equally stiff legs down to the gym anyways to get my desired dose of heavy lifting in. Then, sure enough, halfway through a set of barbell deadlifts, I felt a familiar tearing sensation up and down both sides of my low back, as though someone had ripped a curtain across both sides of my backside. I immediately collapsed to the ground writhing in pain, and after ten minutes of fruitless foam rolling and stretching, I hobbled out of the gym with a grimace on my face, a deep aching sensation in my hips and back, and a sinking feeling in my heart that I would be out of commission for at least a month.
But that didn't turn out to be the case.
Despite suffering a debilitating back injury that would have hobbled me for weeks if it had occurred a decade ago—prior to my ever-growing knowledge of how to heal an injury fast using modern technologies and biohacks—I was back in action weight training, running, playing tennis, and chasing my kids within just five days.
Here's the deal: the place my mind goes whenever something like this happens, especially when the result is shockingly positive, is to share with you exactly what I learned and what I did to fix the issue. After all, I'm one of those guys who digs into every last nook and cranny to find every solution I can for a problem, particularly for anything regarding the body and brain, and it's one of my passions in life to share exactly what I find with you (very similar to what I shared when I got giardia recently, and when I contracted MRSA before that).
So in this article, you're going to discover how to relieve lower back pain associated with exercise and get back into action fast with my top 10 biohacks. You'll also learn exactly why the back can get so screwed by deadlifting in the first place. The first part of this article is edited by me with a few of my practical additions, but mostly penned by my recent acquaintance Daniel Braun, NFPT-CPT, who is the founder of Brawn Body Training Holistics. Dan is currently a fourth-year graduate student in Lebanon Valley College’s doctorate of physical therapy program and has completed extensive anatomy coursework, including a rigorous 6-week cadaver anatomy dissection. He is the author of the Lebanon Valley College’s EXSC 202 Training and Conditioning Practical Manual, which is currently in the publication process. He graciously offered to fill us in on the issues so many of us experience with deadlifts.
After Dan fills us in, we'll then jump into the biohacks I used to fix my own back pain fast. Let's do this!
Why Deadlifting Can Injure Your Back (& What You Can Do About It)
Many trainers and strength coaches often program the deadlift for its incredible ability to activate muscles throughout the body. The deadlift can be loaded heavier than almost all other exercises and has incredible functional carryover.
Yet, deadlifts can also cause serious injury in an instant, typically in the back—very similar to what Ben recently experienced. Before we dive into how a deadlift could cause such debilitating back pain so fast, let’s take a deeper dive into the anatomy of this particular movement.
The deadlift primarily demands hip hinge mobility. Looking at major muscle involvement from the top, the trapezius and rhomboids are active to stabilize the joints of the shoulder girdle.
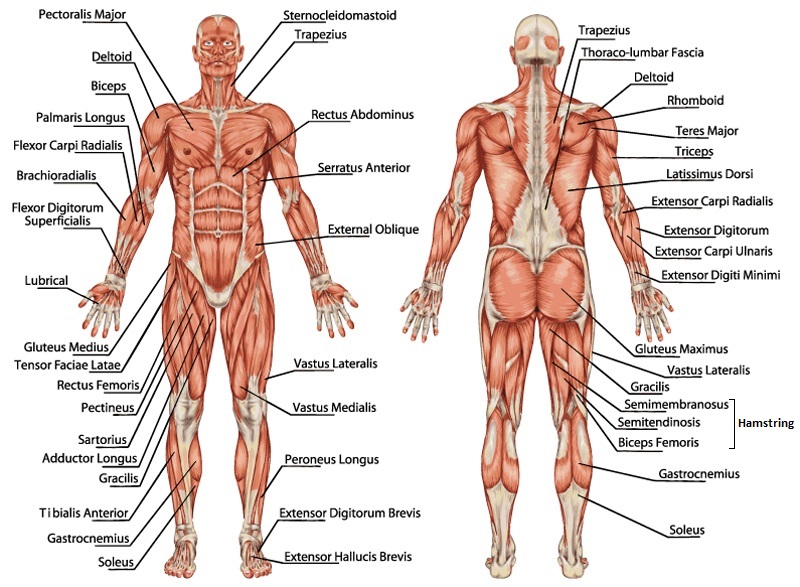
Yep, it starts with your shoulder—you can't deadlift properly with weak shoulder stabilizers, especially if you don't want added strain on your hips and low back.
Next, the latissimus dorsi is vital for shortening the moment arm during the deadlift to give you more leverage, in addition to assisting in stabilizing the spine through numerous axial attachments, such as the thoracolumbar fascia, spinous processes of T7-T12, iliac crest, and inferior 3-4 ribs, and inferior angle of the scapula.
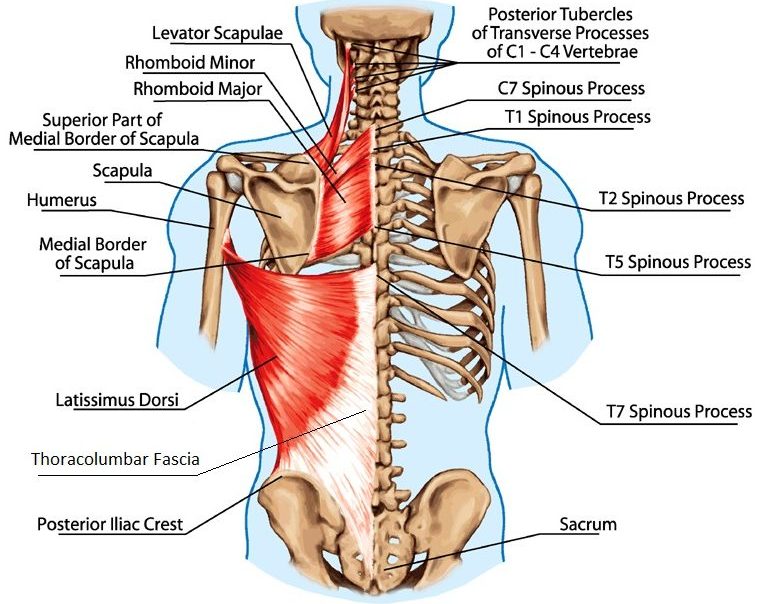
The erector spinae group, consisting of the spinalis, the longissimus, and the iliocostalis, are literally—as you can probably imagine—vital in maintaining a straight spine throughout the lift.
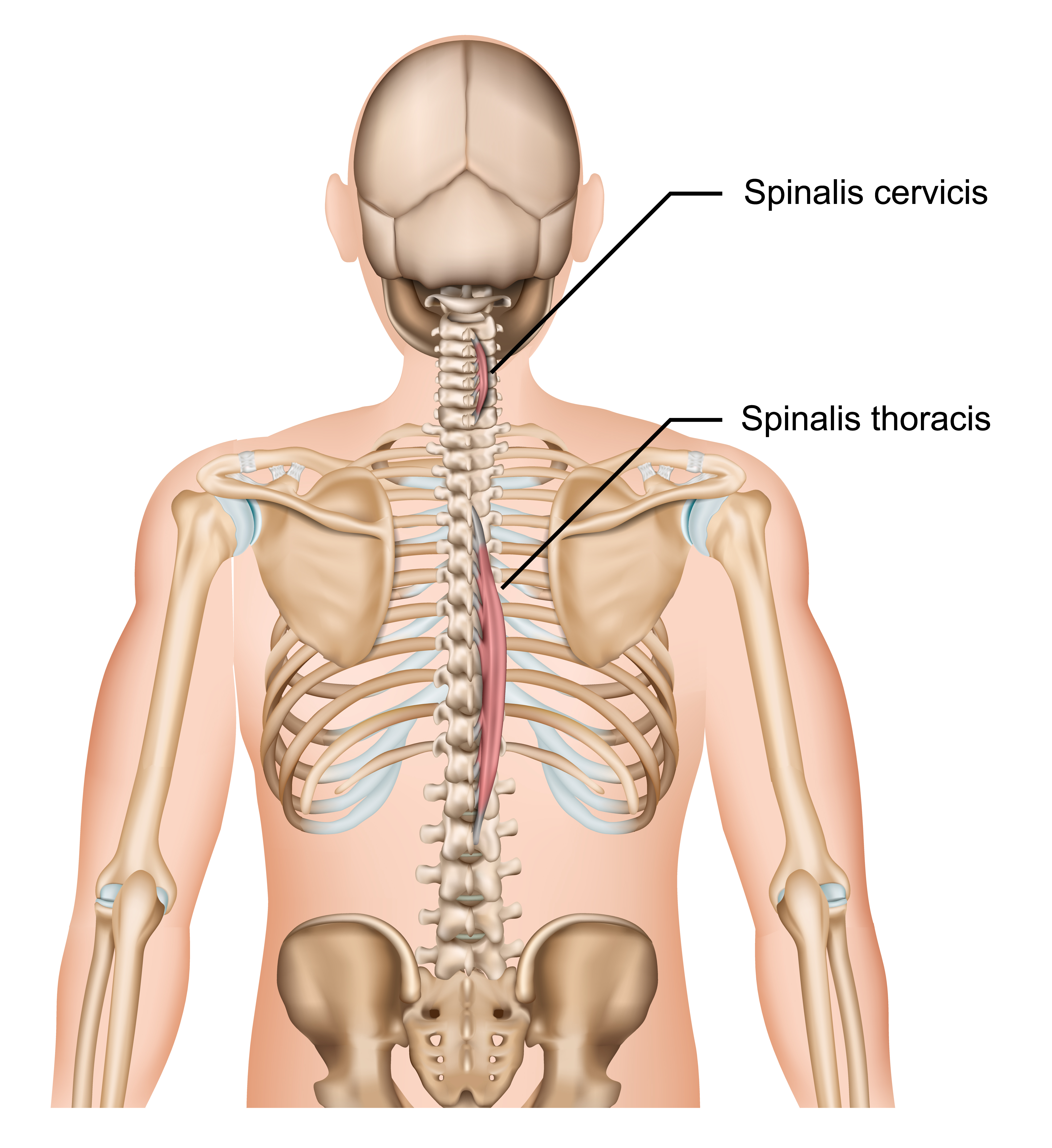
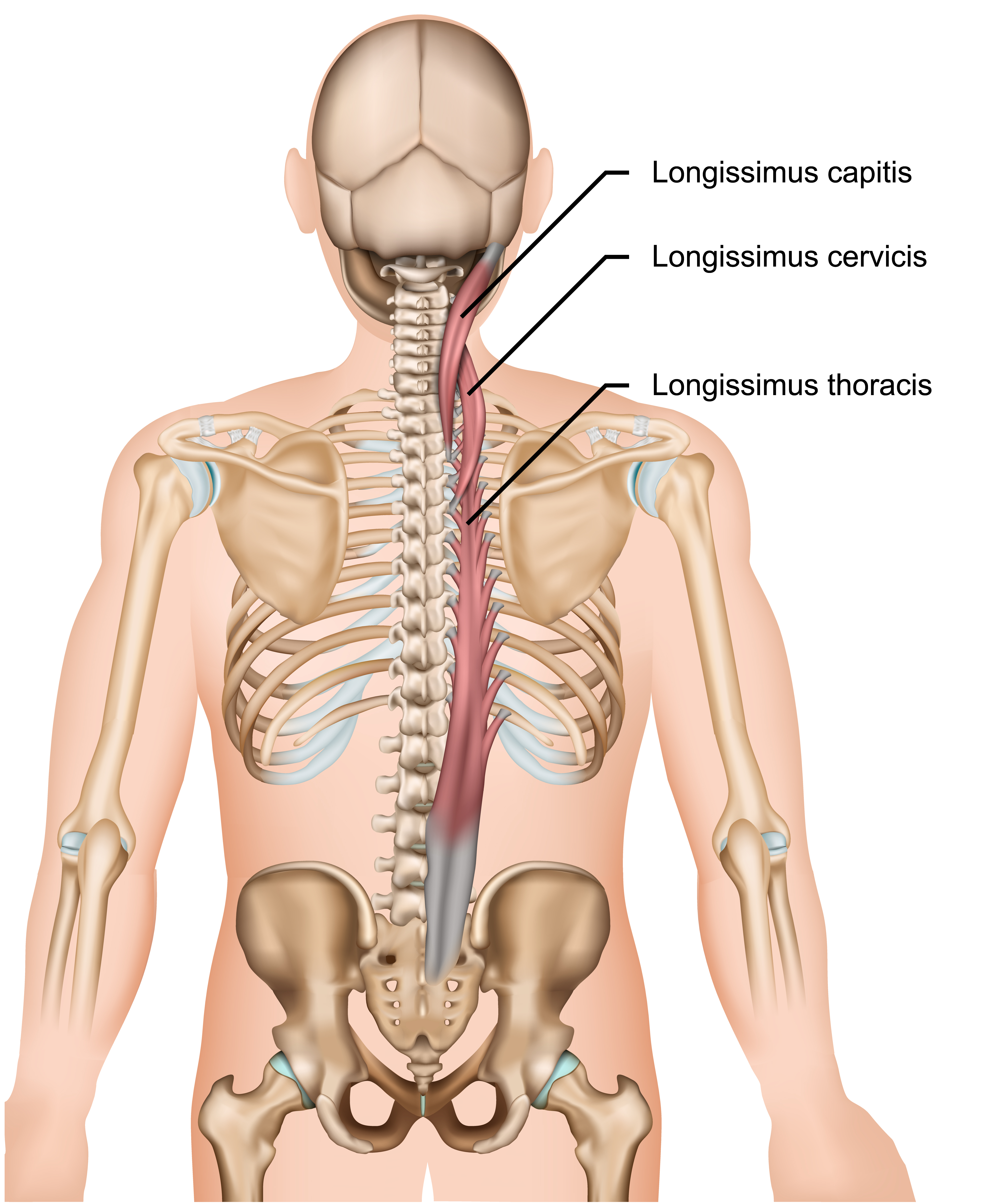
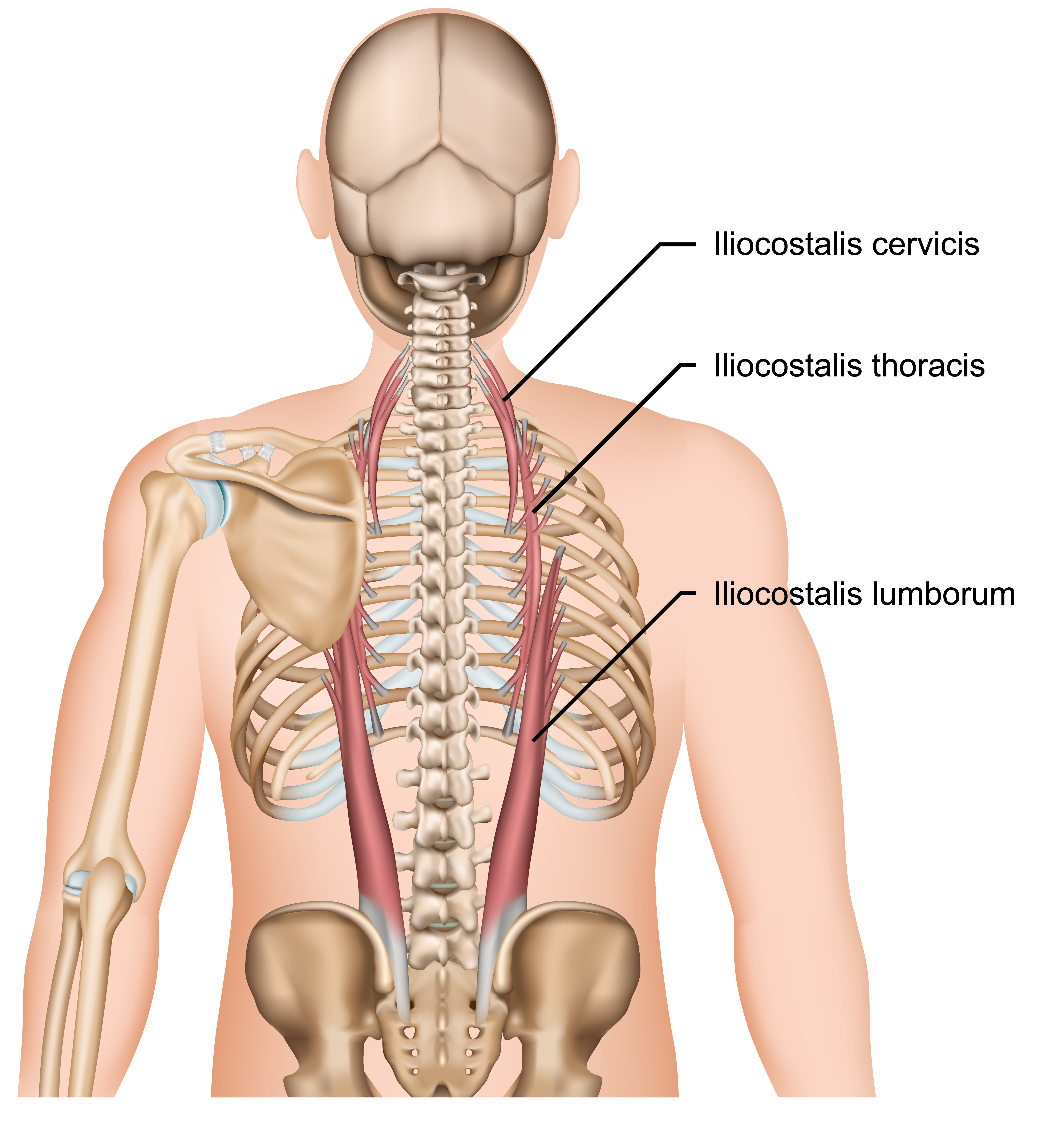
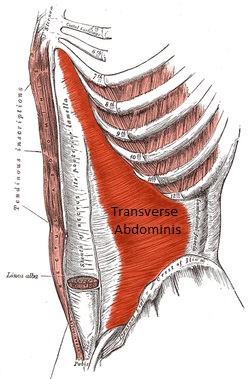
The core muscles, specifically the transverse abdominis, are also vital in performing stabilization in an antagonistic manner that opposes the erector spinae.
The transverse abdominis, that muscle deep in your lower abs, attaches to the thoracolumbar fascia posteriorly and its contractility plays a key role in deadlift performance. In other words, loose stomach muscles, pelvic muscle inhibition and abdominal bracing issues are all key components that may set you up for a deadlift injury.
At the hip, you should note the importance of hip extension in the deadlift, performed by the gluteus maximus, hamstrings, and part of the adductor magnus. The gluteus maximus also performs hip external rotation, which explains why a wider stance “sumo” variety of a deadlift typically results in more gluteal activation, and why you've got no business deadlifting if you haven't first learned how to properly activate your glutes.
The knees are flexed slightly during the setup phase of the deadlift, and therefore recruitment and contraction of the quadriceps are also required during the deadlift to properly extend the knee. But the activation of the hamstrings is significantly greater than the quadriceps during the deadlift due to the ankle and knee moment, which is vital since hamstring utilization can help protect your anterior cruciate ligament (ACL).
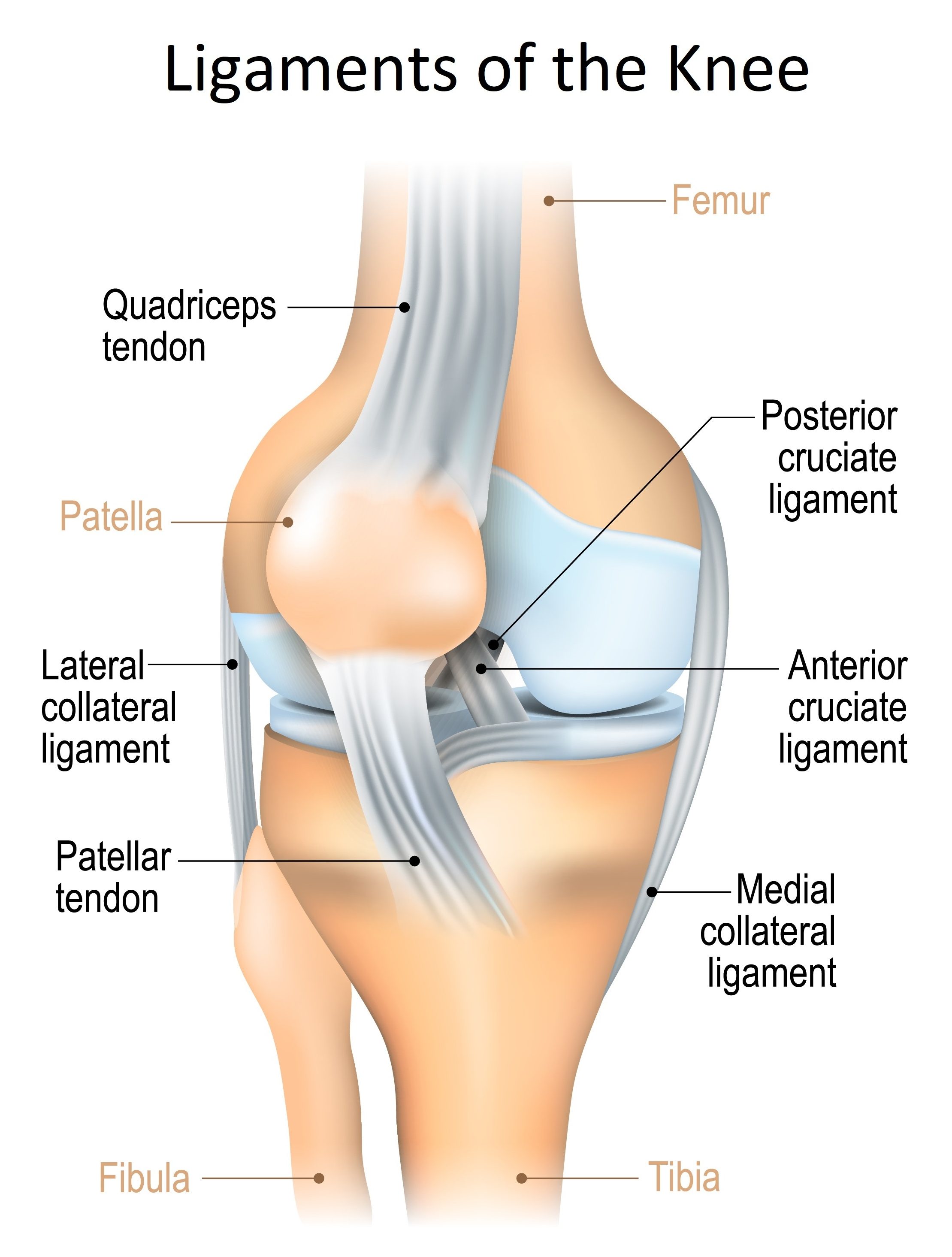
Whew!
Who knew picking up an object could be so complex?
So how does this muscular knowledge apply to reducing your risk of low back pain or injury during the deadlift? Here are four reasons why issues with the muscles listed above can screw you over when it comes to deadlifting.
1. Being Sedentary (Especially Sitting) Affects Pelvic Alignment.
We live in an age where sedentary time continues to increase. With that comes tight hip flexors, tight erector spinae, and weakness in the glutes, hamstrings, and abdominals—three vital muscle groups for the proper execution of a deadlift. The gluteal region specifically receives less blood supply due to sedentary time, and therefore the glutes may not fully recover from exercise due to the lack of nutrient supply, receive poor neurological connection (nerves need nourishment), or be susceptible to pressure ulcers. Inhibition and weakness in the glutes are a hallmark sign of low back pain.
Adding to this issue is Wolff’s law, which states that bones adapt to the forces applied to them. When the pelvis tilts anteriorly due to tight hip flexors and erector spinae, the lumbar spine exhibits an increase in lordosis depth. Increased lumbar lordosis is associated with vertebral body and intervertebral disc wedging, in addition to spondylolisthesis and spondylolysis.
With all this occurring, is performing a high-weight deadlift, which increases activation of the erector spinae and places the pelvis into an anterior tilt, a good idea?
In Ben's case, it really wasn't sitting for a long period of time that caused his pelvic alignment issues, but more likely, being hunched over in a time trial position on a bike the day prior—or possibly even a visit to the toilet just prior to the gym without stretching the hip flexors afterwards (we all do yoga hip openers after we take a long poop before we hit the gym, right?)! As you can see, the message is clear: don't deadlift if you've got short hip flexors, whether the shortening is acute or chronic.
To summarize: high sedentary time causes poor pelvic alignment and tightness in certain muscle groups, causing a variety of nightmare situations for the low back.
2. Being Sedentary Affects Liquid In Your Discs.
When a disc is herniated, the annulus fibrosus will break or tear, causing the nucleus pulposus, the liquid portion of the disc, to be squeezed out. This fluid leaking from the disc can impact a variety of different nerves.
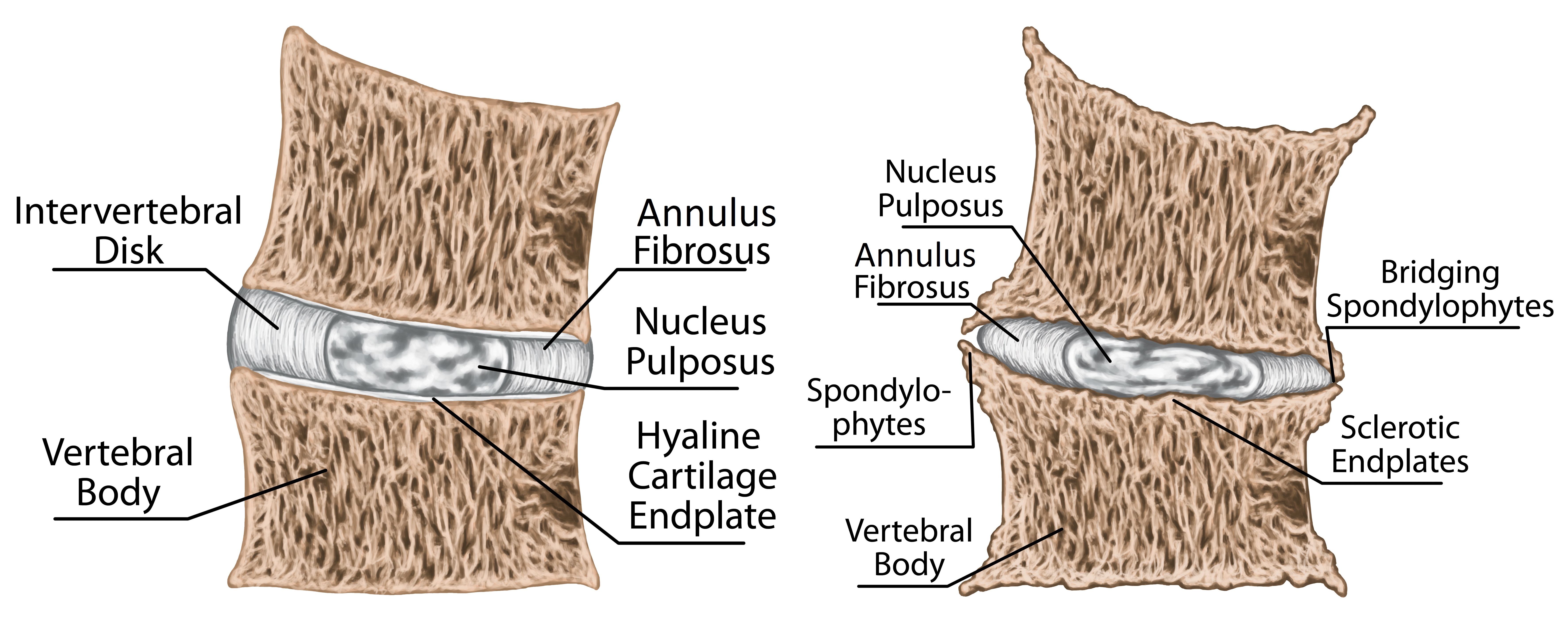
What could be a potential culprit for an acute disc herniation during a deadlift? Once again, we return to the evil of sedentary time. Just one hour sedentary will change the properties of the intervertebral disc in the lumbar spine. These changes result in sudden buckling in the lumbar spine, with a load being applied suddenly to the posterolateral portion of the disc, the site of disc herniation.
This study suggests that mechanical changes in the disc resulting from sedentary time cause instability, increasing the risk for a herniation. Repetitive lifting, specifically lifting objects off the ground (aka, deadlift)—especially after sitting—is a risk factor for herniated discs, which can cause a variety of sensations such as pain, weakness, and numbness/tingling.
3. Muscular Imbalances Increase Risk For Low Back Injury While Lifting.
Remember all those muscles I discussed earlier? What happens when we see one side of a trapezius, lat, erector spinae, hamstring, etc. exhibiting significantly more size and strength than the other? From the last seven years I’ve spent in the gym, I’ve found that very few individuals check their back musculature for asymmetries. It’s too hard for them to see, right? Taking the right lat for example. If the right lat, which shortens the deadlift moment arm, is tighter/stronger than the left lat, the moment arm will be shorter on the right side. When this occurs, we expect a rotational dynamic to occur on the axial skeleton while deadlifting, which in short, is a recipe for disaster.
If you always brush your teeth with your right hand, swing a tennis racquet with your right hand, seem to have better balance when standing on your right foot, or have more grip strength in your right hands, and haven't had a Functional Movement Screen (FMS) ever performed on yourself, I highly recommend you get it done. Click here for a list of FMS practitioners near you.
4. Eccentric Lowering During The Deadlift Increases Muscle Damage.
An eccentric contraction will produce greater muscular damage than a concentric contraction due to maximal force generation, and thus, an eccentric contraction will increase delayed onset muscle soreness, or DOMS. Looking back at our deadlift anatomy lesson, you may recall the importance of the transverse abdominis in the stabilization of the spine through its connection to the thoracolumbar fascia. Poor activation of the transversus abdominis (which would result in the DOMS period due to the extreme muscle damage) is linked to low back pain. When combined with lowering of the bar, this can spell disaster for the low back.
God forbid you ever be deadlifting at any gym that frowns upon rapidly lowering the bar or clunking the weights, because that's going to make the problem even worse, especially if you haven't learned how to properly stabilize your core while lowering a bar to the ground.
In summary…
- Know your anatomy and you can solve a variety of fitness problems! Most of them relate directly to anatomy. It's not that difficult to pick up an anatomy book or even a handy title such as “Becoming A Supple Leopard” and get to know which muscles are where. This helps you know which muscles you need to strengthen or mobilize, and which muscles may need some TLC if you do injure your back deadlifting (hint: it's each of the muscles mentioned above, particularly the hip flexors, hip extensors, back flexors and back extensors).
- Proper pelvic alignment is incredibly important for preventing/treating back pain, and sedentary time has a negative impact on pelvic alignment. Don't sit for long periods of time, and if you have been doing that or, say, riding a bike or taking a poop, stretch your hip flexors and mobilize your hips before hitting the gym.
- Intervertebral discs are impacted by sedentary time, and this can increase the risk of a herniated disc. Once again, overall sedentary time, especially in a seated position, should be limited as much as possible. Even if you're on an airplane or in a board room conference meeting, you can place a rolled-up towel or small bag behind your low back to lessen the shortening impact on the hip flexors.
- Correct muscular imbalances and asymmetries or else improper movement patterns will result. Get an FMS.
- Eccentric training leads to delayed onset muscle soreness (DOMS) due to the increase in maximal force generation, which can lead to back pain due to poor activation of muscles such as the transversus abdominis (damaged muscles will not fire properly). If you want to deadlift and you're in the least bit concerned about hurting your back, drop the bar at the top of the lift.
Final note…
…although the sections above are focused on the pain which can be associated with deadlifting, deadlifts should not be avoided or skipped entirely! I could write about countless benefits to heavy deadlifting, and how important lifting a heavy object is. Just ensure the lift is done safely utilizing the correct form. Modified equipment (i.e. using a hex bar, or elevating a bar into a rack pull position by lifting the bar from a position on which it has been elevated) can be used to continue loading if a full range of motion or limitation is identified. The goal should be a full range of motion, pain-free deadlift, due to the functional importance of the hip hinge movement pattern.
How To Relieve Lower Back Pain Associated With Exercise: 10 Biohacks To Get You Back On Your Feet Fast
Thanks, Dan!
Okay, Ben here again.
Look…I get it: not everybody has a bunch of the biohacks I'm about to describe below at their beck and call in their basement like I do at my Batcave compound in the middle of the forest in Washington state.
But it really would be cool to see more progressively-minded practitioners incorporating these type of therapies and technologies into a traditional physical therapy or sports medicine practice so that these type of things might be available in any city for anybody to do if they want to get rid of back pain (or any other similar injury) more quickly without medications or surgical interventions—very similar to how folks such as CognitiveFX and ReviveCenters have done for concussions and TBI.
So, that being said…
…in addition to walking thirty to sixty minutes per day at a brisk pace; light, easy swimming; yoga; and low-intensity weight training using primarily weight machines at the gym, I used the following protocol to biohack my back pain and return back to function far faster than I used to in my old “pop an Advil and get on a heating pad” days. In my case, this injury had me on the floor of the gym writhing in pain on a Sunday morning, and I was pain-free and lifting weights again by that following Friday, just five days later.
Biohack #1: Topical Muscle Relaxant/Anti-Inflammatory
Your back and hips are going to be spasming like crazy after the injury, and topical magnesium seems to work best for relaxation effects in this department. I personally used Ancient Minerals magnesium lotion with MSM. There is some research on MSM for its relatively effective anti-inflammatory action, and it seems to work quite well when combined with magnesium.
 Here's the ingredients: Water, Genuine Zechstein magnesium chloride, methylsulfonylmethane (MSM), organic vegetable glycerin, organic simmondsia chinensis (jojoba) seed oil, squalane (olive), cetearyl olivate, sorbitan olivate, organic cocos nucifera (coconut) oil, glyceryl stearate, cetyl alcohol, organic butyrospermum parkii (shea butter), xanthan gum, lactobacillus ferment, cocos nucifera (coconut) fruit extract, sodium hyaluronate. Every ingredient scores 1 on the EWG Skin Deep Database (safest on their scale of 1-10).
Here's the ingredients: Water, Genuine Zechstein magnesium chloride, methylsulfonylmethane (MSM), organic vegetable glycerin, organic simmondsia chinensis (jojoba) seed oil, squalane (olive), cetearyl olivate, sorbitan olivate, organic cocos nucifera (coconut) oil, glyceryl stearate, cetyl alcohol, organic butyrospermum parkii (shea butter), xanthan gum, lactobacillus ferment, cocos nucifera (coconut) fruit extract, sodium hyaluronate. Every ingredient scores 1 on the EWG Skin Deep Database (safest on their scale of 1-10).
Biohack #2: Rumble Roller + “Peanut” Roller + PSO-Rite Device
Every morning, I specifically rolled up and down and sheared back and forth my quadratus lumborum, gluteus medius, gluteus minimus, psoas, iliacus, IT bands, and adductors. I also ran a peanut-shaped roller up and down the vertebra of my low back, then used a PSO-Rite device to dig deep into and release my psoas (the handle of a kettlebell also works quite well, but only if you have the pain tolerance of a child-bearing mother).
You can get the Rumble Roller, the “Peanut” roller here and the PSO-Rite device here.
Biohack #3: Inversion
Inversion is just a form of “traction,” and in this case, spinal traction is a form of decompression therapy that relieves pressure on the entire spine, and opens up the hip flexors too. Spinal traction is often used to treat herniated discs, sciatica, degenerative disc disease, pinched nerves, and many other back conditions. For this, I used a YogaBody Yoga Trapeze that hangs from my living room balcony, but Teeter Inversion tables or a set of gravity boots are also very good. I did some form of spinal traction for three to five minutes, several times per day—especially after sitting.
You can get the YogaBody Yoga Trapeze here, the Teeter Inversion table here, and an EZ-Up Gravity Boots here.
Biohack #4: The “Coil” Stretch
Although I started each day with fifteen minutes of yoga hip openers, similar to these, of all the stretches I incorporated, my friend David Weck's “coiling stretch” seemed to the most effective to utilize throughout the day, especially every time I had a quick break from work. I simply held the stretch for ten seconds each side, three times through, multiple times during the day. The stretch itself is a bit difficult to explain but seems to open up the hip flexors and back muscles like gangbusters. You can watch a video of the stretch below, and listen to my podcast with David here.
Biohack #5: Pulsed Electromagnetic Field Therapy (PEMF)
PEMF machines generate a magnetic field that passes through the skin into the underlying tissue and can relax capillary walls, thereby boosting blood flow to the painful area. PEMF can also help prevent the muscle spasms that accompany many forms of pain, especially low back injuries, by interfering with muscle contractions. The frequencies may also interfere with the electrochemical reactions that take place within nerve cells, impeding their ability to transmit pain messages to your brain. I own a Pulsecenters PEMF pad, and did this exact protocol at least once per day:
Biohack #6: Grounding Patches
 You can click here to listen to my recent podcast with Clint Ober, in which we discuss the little known tactic of grounding (also known as earthing) to reduce inflammation and accelerate healing. For this, I used the grounding patches in Clint's Ultimate Longevity website. I put them on the whole day while working at the standing workstation in my office, for at least 20-30 minutes each time: one on front of hips and one on lower back as close to the area of pain as possible. This type of “spot treatment” works better than laying on a ground mat. Grounding not only reduces pain, but also alters the numbers of circulating neutrophils and lymphocytes, and can affect various circulating chemical factors related to inflammation.
You can click here to listen to my recent podcast with Clint Ober, in which we discuss the little known tactic of grounding (also known as earthing) to reduce inflammation and accelerate healing. For this, I used the grounding patches in Clint's Ultimate Longevity website. I put them on the whole day while working at the standing workstation in my office, for at least 20-30 minutes each time: one on front of hips and one on lower back as close to the area of pain as possible. This type of “spot treatment” works better than laying on a ground mat. Grounding not only reduces pain, but also alters the numbers of circulating neutrophils and lymphocytes, and can affect various circulating chemical factors related to inflammation.
You can get the same grounding patches I used here.
Biohack #7: NanoVi Water
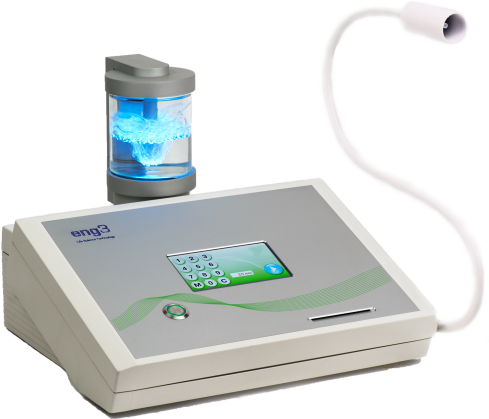 NanoVi is a drug-free approach used to initiate repair and rejuvenation by improving cellular activity. The NanoVi is a device that infuses water with an electromagnetic charge that generates ROS-signaling free radicals to subject your body to mild oxidative stress. By charging the water in its humidifier holding tank, then delivering it through a tube to a nasal cannula around your nose or a small pipe you can breathe from, the NanoVi creates a “bio-identical signal” that closely resembles the signal closely resembling the one given off by the free radicals within your body. This stimulates a stronger healing response than the signaling free radicals alone would cause, resulting in an improved response to oxidative stress and enhanced cell repair and recovery. Of all the “hacks” I used, this is one I didn't directly “feel” while using it, but I'm just trusting the research on this one, and would love to see some kind of human clinic study eventually emerge that shows the actual impact on tissue inflammation. Regardless, I included it and breathed the water for about an hour a day while working in my office. Click here to listen to my podcast with the folks at NanoVi and learn how to get one of these devices for yourself here.
NanoVi is a drug-free approach used to initiate repair and rejuvenation by improving cellular activity. The NanoVi is a device that infuses water with an electromagnetic charge that generates ROS-signaling free radicals to subject your body to mild oxidative stress. By charging the water in its humidifier holding tank, then delivering it through a tube to a nasal cannula around your nose or a small pipe you can breathe from, the NanoVi creates a “bio-identical signal” that closely resembles the signal closely resembling the one given off by the free radicals within your body. This stimulates a stronger healing response than the signaling free radicals alone would cause, resulting in an improved response to oxidative stress and enhanced cell repair and recovery. Of all the “hacks” I used, this is one I didn't directly “feel” while using it, but I'm just trusting the research on this one, and would love to see some kind of human clinic study eventually emerge that shows the actual impact on tissue inflammation. Regardless, I included it and breathed the water for about an hour a day while working in my office. Click here to listen to my podcast with the folks at NanoVi and learn how to get one of these devices for yourself here.
Biohack #8: Infrared (Sauna + Biomat + JOOVV)
Red light therapy can alleviate chronic inflammation by increasing blood flow to the damaged tissues, and it’s been found in numerous clinical trials to increase the body’s antioxidant defenses. Dr. Michael Hamblin of Harvard Medical School and Massachusetts General Hospital is one of the world’s leading photomedicine researchers, and he's studied light therapy at length, concluding that one of its most reproducible effects is “an overall reduction in inflammation, which is particularly important for disorders of joints, traumatic injuries, lung disorders and in the brain.”
Dr. Hamblin explains that wavelengths of natural red and near-infrared light are “a very mild form of stress that activates protective mechanisms in the cells. For instance, when longer wavelengths or visibly red light hits the skin, it nudges mitochondria to make energy more efficiently and boost production of healing anti-inflammatories or disease-fighting antioxidants.”
Based on this, I used a full-body JOOVV light panel for 10 minutes per day while working in my office, with my shirt off for direct exposure to the back. I did the same on the front of my body to hit my hip flexors and transversus abdominis. In addition, anytime I was in bed or laying down, I did so on the Biomat, which also produces infrared.
Finally—and this was a big game-changer due to the combination of heat—activation of the parasympathetic nervous system, and infrared, I did as much stretching as I could in my infrared sauna, including all the hip openers and coil stretches mentioned earlier in this article, and also quite a few Core Foundation stretches (click here to get the book “True To Form”, which teaches you all these stretches, which are fantastic for decompressing the spine).
For the JOOVV, I used the Elite Panel, for the Biomat, the Biomat Pro, and for the sauna, the Clearlight Sanctuary Model.
Biohack #9: BPC-157 Peptide
There is a large body of research on the efficacy of the injectable or orally administered peptide BPC-157 on tendon healing, quelling of inflammation and increased blood flow to injured areas. I used a relatively large bolus of BPC-157: 500mcg every morning for five consecutive days, and although it's available systemically wherever you inject it or even with oral administration, I decided to just subcutaneously inject directly over the quadratus lumborum on both sides of my back, where the pain and stiffness seemed worse. You can learn more about BPC-157 and how it (and other peptides) works in this article and also in this podcast with Dr. William Seeds and this podcast with Jean-Francois Tremblay.
You can get Dr. Seed's Oral BPC-157 here (use BEN for a 15% discount), and check the International Peptides Society website to find a knowledgeable physician who can prescribe you the injectable form.
Biohack #10: Kion Flex
Kion Flex is a combination of multiple factors that can support faster injury recovery, including:
- Turmacin® – You’ve heard of curcumin, but what about turmerosaccharides? Turmacin is the first water-soluble extract of turmeric to contain turmerosaccharides, which support a balanced inflammatory response to physical activity and have unique benefits for joints.
- AyuFlex® – AyuFlex is a non-GMO, organic extract of the Ayurvedic superfruit, Haritaki. It has unique joint health benefits that can support whole-body joint function and help you move more freely.
- Proteolytic Enzymes – Enzymes are biological catalysts that speed up chemical reactions in the body. When taken at the effective dose, certain blends of enzymes can facilitate the recovery process and help you bounce back faster from your daily activities.
Ultimately, this stuff is like a “shotgun formula” of all the herbs and compounds that can assist with speedier injury recovery, and I simply popped twelve (yes, twelve!) capsules per day on an empty stomach, just prior to bed. You can get Kion Flex here.
Summary
So that's it.
Obviously learning how to relieve lower back pain comes down to plenty more than a simple heating pad and a handful of ibuprofen, and I hope the tips in this article have been helpful for you. Admittedly, I only scratched the surface of the full range of recovery modalities that I consider to be far more progressive than the ho-hum recovery advice you might get from the average physical therapist or physician, but fear not…
…my upcoming book “Boundless” has an entire, very “meaty” chapter dedicated to recovery and injury healing. You can click here to get on the list for immediate notification when that book gets released.
Again: I fully realize that not everybody has most of the stuff listed above just lying around their house, but I'm keeping my fingers crossed that physicians and practitioners who might read this article consider adding some of the elements above into their practice. I've found that many of these, although they fly under radar, are incredibly beneficial in my own injury recovery and healing process, especially when “stacked” together.
In the meantime, leave your questions, comments, and feedback about biohacking back pain below, or your own tips, and I promise to reply!
























It usually comes down to doing the right exercises, stretching and having gear that is appropriate for your needs. To help with this process I always research products before purchasing them so as not only can you get a good quality product but also avoid injuries by using it correctly from day one!
Hey Ben, My X-ray reveals mild spondylitis in the lower spine, Do you have any tips to reverse it?
I’m replying sort of in response to the disparaging remarks regarding the price. Ben is recommending this stuff because it works. To make it accessible, many have come up with a communal or club-type model of varying degrees of expense that grant you access to such equipment. You might search for one in your area. Often this “stuff” is sprinkled across a metro area among many practitioners an wellness centers. You might go to the equipment company websites via ben’s link click for locations/practitioners or call the number given and ask for a location in your area. Try searching for “nanovi” and your state or Pulse PEMF and your state or city.
Thank you for a useful article and a useful list of new items. I have long been thinking about how to make my training more effective and minimize various injuries. Most often, it comes down to proper exercise, stretching, and good equipment and clothing. I often read reviews before buying to get the best sports products
Hi Ben,
Thanks for sharing all of this information. I injured my lower back doing deadlifts over 6 years ago and I have had chronic back pain/sciatica ever since. I have tried everything from chiropractic, PT, inversion therapy, medication, injections, the PSO rite, MSM, and even had surgery in 2015 but am still having the issue. What do you think would be the next best option for me? My last MRI confirmed that I have 2 herniated discs in my L4/L5 and L5/S1. Thanks in advance!
-Joe
These injuries are very painful. I remember my first sprain of the back ligaments, it was very painful. I think that you need to be very careful during the exercise, so as not to get terrible injuries
Many exercises can somehow damage your muscles and you may feel pain. You should understand that sports injuries often happen, even if you know the safety of exercise well.
I think that in such cases, you need a rest or CBD oil, for example
Hey Ben, big fan here.
I’ve had a fascia problem for a couple of months now and was curious about how you would deal with this in my situation. What would your protocol/approach be like?
Quick story. About 2 years ago ( I’m 22 now ) I joined the gym and followed an internet fitness program by myself, without the help from professionals. And to summarize it, it was like a powerlifting protocol, it was all about getting those personal records. I did not stretch, I did not work on my mobility, no warm-up, I didn’t even know what a foam roller or fascia was or anything about recovery really.
And so, a couple of months ago I started noticing that my muscles started to get very tight, all around my body. And because at the time I didn’t know anything about it really I ignored it and kept going. Which only made it worse, even tighter.
And so, it’s been 2 weeks now since I’ve been doing some deep tissue work following Kelly Starret “TheReadyState” app and foundation training every day and I’ve seen some improvements BUT it looks like it’s gonna take a couple of months to really become fully mobile again. So my question is, What would your days/protocol would look like to solve very tight muscles? Your top recommendations,
And thank you, really appreciate the value your putting out there into the world.
You can watch my entire mobility routine here: https://www.facebook.com/BGFitness/videos/morning… Additionally, I'd be happy to help you via a one on one consult. Just go to https://BenGreenfieldFitness.com/coaching to learn more.
Hello, Ben! Another great article!
I have liked the foam rolling morning routine. May I as, what kind of rumble roller would you recommend? Harder or softer? Mostly for legs massage and upper back as well.
Thanks!
Probably the blue. The black one (extra firm) is for experienced users with very dense muscle tissue that doesn't respond to typical massage pressure. https://bengreenfieldfitness.com/ben-recommends/g…
For a cheaper and marginally slower.
I normally go to number 1 (but instead making turmeric, boswellia and black pepper soaked tissue pads and using topically) for a start, then as soon as first stage inflammation goes down start adding gentle re-configuration of movement patterns. E.g. Slow Locomotion, DNS techniques.
However I think number 4 would be great combined with this: http://josephbartz.de/essays/en/waves.html – A must in my books for re-learning spinal locomotion patterns.
Hi Ben,
What is your take on the recent vaping related illnesses?
How limited should someone be vaping CBD and THC a few times per week, should I be worried?
Chiropractic is proven to be a the top of list in dealing with this. Most Chiro’s have decompression, laser, supplements, lotions and potions, rollers, K-tape, exercises, e-stim, and 8 years of education to walk you through this. Or you spend thousands and try to figure it out yourself.
I agree Jim G! Chiropractic to biohack your body recovery.
Too bad most Chiropractors are uneducated scam artists. Their schooling is a abysmal.
Lquinta, you can’t argue with the stats, especially for back pain. Chiropractic works for low back issues.
More expensive BS most of us working class people could never afford!
So all you need to do is spend around $15,000 and 6hrs a day and you to could heal your back pain in 5 days instead of 4 weeks. 🤔
I’ve been dealing with some similar issues and find the trap-bar deadlift (standing on blocks to increase the range of motion) seems to put much more even (front-to-back) stress on the spine. I’m hoping to re-start on the standard deadlift but i’m increasingly thinking the trap-bar deadlift is a better long-term risk/reward option.
I absolutely agree that the trap bar can be very beneficial. I have a natural anterior pelvic tilt due to genetics and weaker transverse abdominals, and I have always struggled to effectively activate the abs when using a standard Olympic bar to deadlift. About 6 months ago, I relegated myself to using only the trap bar for deadlifting – and since then, my max has improved significantly, my abs feel much more involved in the movement (confirmed by severe DOMS a day or two later), and my lower back pain is gone!
More like wallet hacks