May 4, 2015
I once heard a sleep researcher amusingly describing sleep as a “condition” that a physician describes to parents of a newborn child.
The story goes like this:
A pediatrician presents a brand new baby girl to her parents and reports to them that the child is healthy, but to please beware as new parents that…
…”frequently your baby will go unconscious and unresponsive to normal stimulation. The frequency of these attacks will gradually decrease to just one-a-day by the time she goes to school, but that will last throughout her life. Periodically once unconscious she will be paralyzed except for spastic muscle twitches, her eyes will dart back-and-forth, and her heart rate and breathing rate will get irregular. As she gets older she will have hallucinations during these episodes. She will hear voices and see things that aren't there. Some of these things will be very strange and maybe even terrifying causing her to sit up and other times scream out in freight. But not a problem, because this condition is also characterized by total amnesia, so she won't remember any of these terrifying experiences, including the loss of consciousness, paralysis, spastic muscle contractions, cardiorespiratory arrhythmia, or hallucinations.”
And then the physician reveals the exact “terrifying” condition he is describing. Did you guess it?
That's right: it's sleep.
The parents were of course relieved to learn that their baby's condition was merely that of sleep. But hearing this description of sleep hopefully gives you insight into the fact that physicians and medical researchers actually know very little about why we actually sleep, and have little understanding of what really happens to us during sleep.
The phenomena of sleep is both loved and hated by the modern American. Look at many of the common catch phrases that have been indelibly etched in the modern psyche, including…
“Sleep is a symptom of caffeine deprivation.”
“I can sleep when I am dead.”
“Sleep is a luxury I can’t afford.”
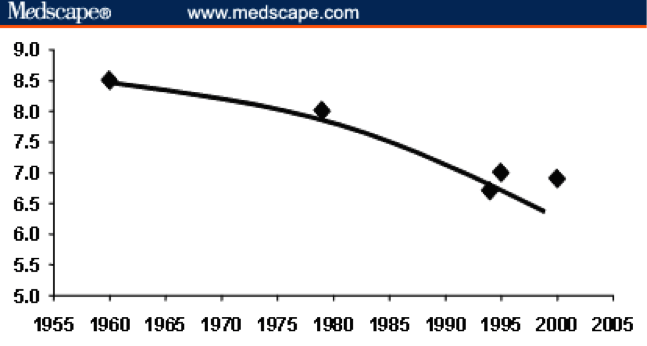
The CDC reports that 30 percent of adults admit to less than 6 hours of sleep a night. The myth of getting by with less sleep to get ahead has been around only a short time though, since the early 1900s. The graveyard shift was invented to ramp up manufacturing during World War II. Thomas Edison, a notorious short sleeper, famously described his optimal day as working for 18 hours a day and getting by with 4 to 5 hours of sleep per night. In comparison, in his era, the average American slept just over 8.5 hours a night.
It is amazing how quickly our priority for sleep has eroded. Some medical researchers have found a connection with increase in autoimmune disorders, in part due to the lack of opportunity to restore one’s health through sufficient sleep. But like autoimmune disorders, insufficient sleep is not considered a disease, but rather the body somehow “short-circuiting”, and some kind of a self-inflicted problem. The definition of insufficient sleep is succinct: a neurologic disorder in which individuals persistently fail to obtain enough sleep to support normal wakefulness, and perhaps one day it may include in the definition, fail to obtain enough sleep to optimally support the immune system as well.
Epidemiologists have graphically demonstrated the stark decline in average nightly sleep duration for Americans over the last few generations, in 1950 – 8.5 hours, in 1970 – 7.5 hours – in 2000 – 6.25 hours, and so on.
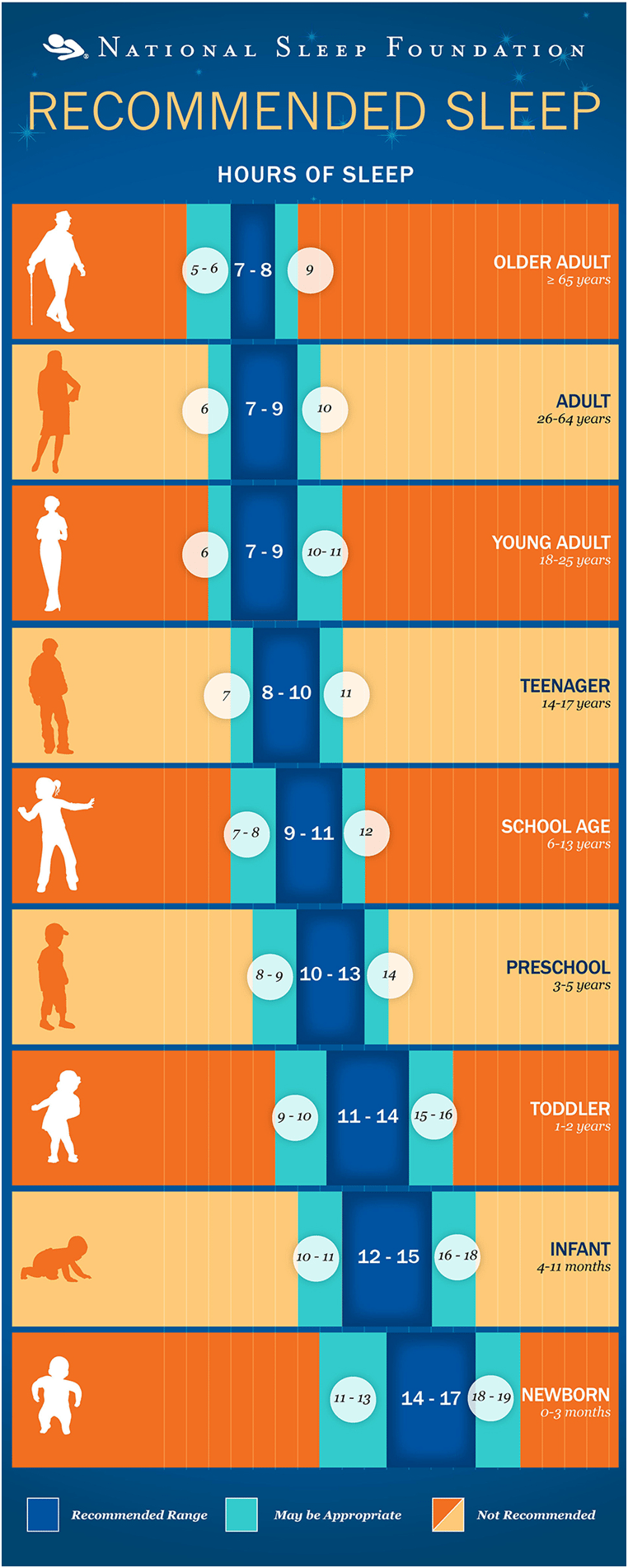
So what does this mean to someone who wants to stay at their peak performance? What has research shown is the detriment of not getting enough sleep? How much does a healthy person, let alone an athlete need to be at their peak? Sure, the average adult may need 7 to 8 hours of sleep a night, but the answer is not that simple, and in an ideal world, you'd be able to quantify what is needed to function at your best.
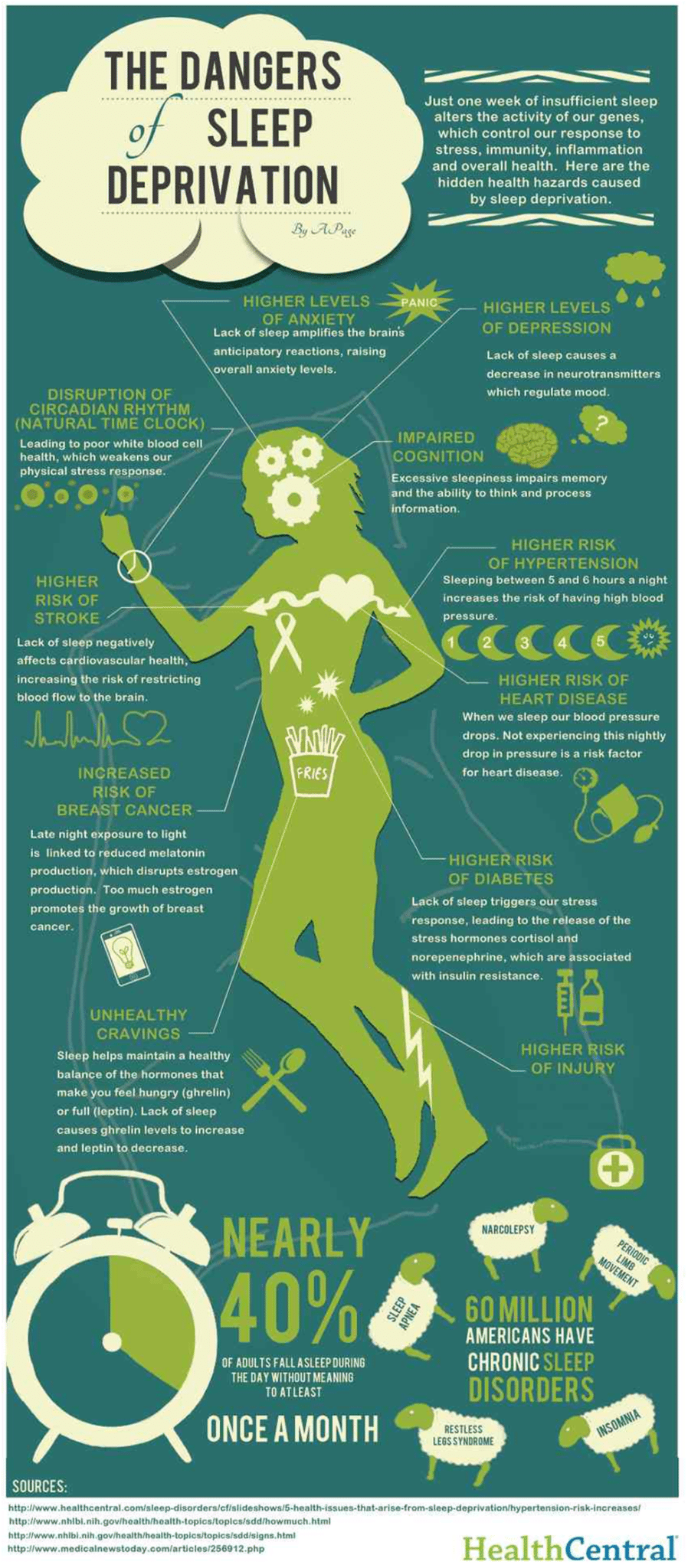
So in this article, you're going to discover what happens to your body when insufficient sleep occurs and new objective ways to quantify if that you're truly getting enough sleep.
—————————————-
Sleep Deprivation and Immunity
Animal studies have demonstrated a sleep-promoting factor contained in the cerebrospinal fluid. This factor is called adenosine. So I always ask my patients…
…what is the most commonly used medication in the world?
I preface by telling them it is neither over-the-counter nor a prescription. The medication is a blocker of adenosine and that medication is caffeine, often in a morning, mid-morning, afternoon, and perhaps mid-afternoon or evening cup of coffee.
But like any medication, caffeine has a toxic dose, and one big reason for this is because it can block adenosine. This is because adenosine is essentially the exhaust fuel of the brain’s metabolism.
Here's how it works: when the glial cells of the brain are running low on ATP (adenosine is the “A” in this adenosine triphosphate) to breakdown from stored glycogen (glucose storage) that 2 ADP (adenosine diphosphate) can be used to make an extra ATP and a leftover adenosine molecule. So excess caffeine intake can actually strip the brain of necessary fuel, especially when glial cell ATP is already low from lack of sleep.
Let's use the case of coffee, ATP depletion and lack of sleep to see how this has a profound effect on your immune system, the development of immunological memory and other inflammatory homeostatic functions.
The immune cascade in response to infection involves the activation of neutrophils, monocytes and macrophages (white blood cells are the soldiers of the immune system). These are the cells that produce inflammatory cytokines (proteins that serve as messengers between cells) such as IL-beta, IL-6, TNF-alpha, which stimulate hepatic production of C-reactive protein (hsCRP is an inflammatory marker used by doctors to predict the risk of heart disease or general inflammation). These cytokines are elevated the morning after as little as a single night of four hours of sleep restriction. Inflammatory mediators participate in the CNS (central nervous system) regulation of sleep. I am hopeful that with time there will be biohacks that may help mitigate the inflammation related to sleep deprivation. But for now the best medicine is simply choosing to avoid the inflammation in the first place.
During experimental sleep deprivation of healthy volunteers, blood pressure and other indicators of sympathetic output have been found to increase. This increase in sympathetic (the fight or flight nervous system) output results in increased pro-coagulatory (blood clotting factors) markers produced by stimulating vascular endothelium (the lining of the arterial wall which normally is extremely slippery when healthy). This alteration can increase shear stresses associated with increased blood pressure, and this can activate inflammatory mediators.
Other data supports a connection with increased pain perception and sleep loss. Inflammatory markers, including prostaglandins and pro-inflammatory cytokines, have been shown to sensitize nociceptors (pain receptors), contributing to the development of spontaneous pain and hyperalgesia (increased pain).
In addition, animal trials have noted reduced bone density in sleep deprived rats. Dr. Everson’s sleep research found rat hematopeotic stem cells are half as effective after 10 days of sleep deprivation. This decreased cell activity was related to impaired migration capability of the bone stem cells.
Human trials have demonstrated with vaccination experiments to assess antibody creation in response to flu vaccine a reduced immunity in sleep deprived subjects. These subjects had ½ the antibody response to vaccine after volunteers were sleep deprived to 4 hours a night for 6 days. This impairment persisted for a full month after recovery sleep was allowed. Natural killer cells attack viruses and tumor cells. Research has found that healthy volunteers subjected to a 4 hours of sleep loss were found to have a 73 percent reduction in natural killer cells.
So from stripped brain fuel, to increased pain perception, to lower bone density, to a reduction in natural killer cells, to an increase in blood pressure and an increase in inflammation, we now know that a lack of sleep has profound effects on your immune system – even if you're able to be awake and function.
—————————————-
Sleep Deprivation and Glucose Metabolism
Current data point to three pathways that link sleep restriction with diabetes risk and obesity:
1. alterations in glucose metabolism;
2. upregulation of appetite;
3. decreased energy expenditure.
The role of sleep in glucose regulation has been recognized for over a decade. Initial studies on sleep curtailment were experimentally testing short periods of total sleep restriction. These studies found that despite significant negative metabolic derangements in hormone and glucose utilization that given the opportunity to have recovery sleep, these derangements were quickly reversed. The human physiology tolerates one night of total sleep restriction well…given the opportunity to catch up. But the more relevant experiments are the ones that test the effect of partial sleep restriction over several days or longer.
The mechanisms affecting glucose metabolism following recurrent partial sleep restriction are believed to be multifactorial. The acute reduction in insulin release could be due to increased sympathetic nervous activity at the level of the pancreatic beta-cell. Cardiac sympatho-vagal (this is the balance between the rest/digest and the fight/or flight autonomic nervous system) balance is affected, as evidenced by reduced heart rate variability when sleep is restricted. Secretion of counter-regulatory hormones, Growth Hormone and cortisol, may contribute to the alterations in glucose regulation noted during sleep loss. Subjects tested during the peak of sleep loss were found to take 40 percent longer than normal to regulate blood glucose levels, and the ability to secrete insulin decreased by approximately 30 percent.
The imbalance of catabolic (biochemical reactions that break down molecules in metabolism) and anabolic (biochemical reactions that stimulate protein synthesis and muscle growth, and insulin) hormones leads to a dysregulation of the arcuate nucleus of the hypothalamus where there is opposing sets of neurons, appetite stimulating and appetite inhibiting.
Epidemiological data show an association between short sleep and irregular eating habits, snacking between meals, excessive food seasoning and reduced consumption of vegetables. The Wisconsin Sleep Cohort Study found evidence that sleep loss may alter the ability of leptin and ghrelin to accurately signal caloric need. This imbalance produces an internal perception of insufficient energy availability despite an increase in caloric intake. Dr. Carol Everson found in rats that were subjected to sleep restriction for 10 days a persistent 20 percent increase in food intake, despite the opportunity for recovery sleep.
The Nurse’s Health Study followed 80,000 women observed an association between sleep duration and Body Mass Index (BMI) where the lowest mean BMI was observed among those nurses reporting sleep in 7-8 hours a night. Recent research was performed on healthy controls that comprised 12 months of 30 minutes of sleep restriction per night. This cumulative sleep debt resulted in increased adipose tissue and insulin resistance. The study results extrapolated that this mild sleep debt increased the risk of obesity by 72% [15].
It's important to emphasize here that cumulative lack of sleep is the issue, and it's a serious issue when it comes to blood sugar control, appetite and fat loss.
————————————————
Sleep Deprivation and Hormones
There is little research on the effect of sleep loss on female sex hormones, but for male sex hormones there is some strong support. Recently, the National Heart, Lung and Blood Institute funded a sleep deprivation trial. This trial was performed on 24 year old males. When deprived of sleep their testosterone levels dropped by 10-15 %. The reason for this drop has been postulated to be related to changes in LH (luteinizing hormone – a hormone produced in the anterior pituitary gland). In light of this new information, one might plan on adding more sleep time to their health regimen and reassess testosterone levels a month later.
Don’t forget the power of melatonin (circadian – 24 hour cycle – sleep hormone) on overall health. Research on the effect of exogenous (supplement form of melatonin) may not have near the same effect as simply adding more sleep to one’s nightly habit. The natural secretion of this hormone initiates a cascade of biological processes. The general public is familiar with melatonin as a sleep related hormone, but many may not be aware of its impact on brain glutathione (a major endogenous antioxidant produced by the cells) and its powerful antioxidant effects. It is considered more powerful than vitamin C, E, A and the carotenoids.
Unfortunately, melatonin is a terminal antioxidant, meaning it does not undergo redox cycling, which is the repeated reduction and oxidation to regain its antioxidant properties. Thus, sleep is required to regenerate this master antioxidant. If sleep is a health promoting process in our 24 hour cycle, then it is logical that a major player in sleep promotion would be a powerful antioxidant.
Here is how it works: when melatonin is produced, it can work as an antioxidant to free up glutathione. Why is this important? When we are low in antioxidant in general or low in any one specific cofactors then glutathione takes on the role of eliminating free radicals. Once this happens, supplies of glutathione become depleted and slows down all the other roles that glutathione plays in the body, including detoxification, DNA repair, antioxidant recycling, mitochondrial energy support and immune system regulation.
The best way to promote sleep physiology relating to melatonin secretion is likely by avoiding light pollution experienced by most people in the evening hours. Avoiding bright light sources, especially blue wave length can support natural production of melatonin in the brain.
—————————————–
Sleep Duration, Genetics and All-Cause Mortality
Finally, meta-analyses of population-based studies looking at the relationship between sleep duration and all-cause mortality reported a 10 and 12 percent increased all-cause-mortality in individuals with habitual short sleep duration.
But does everyone respond the same to sleep curtailment?
Recent twin studies have uncovered some genetic variations that may protect some people from sleep deprivation. The mutations that occur to the p.Tyr362His BHLHE41 gene appear to allow some to tolerate shorter sleep durations and maintain normal alertness and limited signs of inflammation.
Unfortunately, right now the average person is trying to function like Thomas Edison…which won’t end well for most of genetically. My feeling is that Edison is probably one of those folks who may have had the p.Tyr362His BHLHE41 mutation (only an educated guess).
—————————————
Sleep Tips From A Sleep Doctor
Believe it or not, the most powerful non-medication intervention for insomnia is using the naturally occurring soporific neurotransmitters and getting in tune with one’s natural sleep rhythms. The body is made to be awake for approximately 16 hours of the day. This rhythm is entrained to ebb and flow with the natural increase and decrease in hormones throughout the day. If the schedule is interrupted, then the natural cycle of hormones will be disrupted as well, so you ust maintain as normal of a wake time as possible. The reason for this is that if you go to sleep later and have an anchor of wake time, you will likely have more sleep pressure developing throughout the day, but you won’t disrupt the overall sleep/wake rhythm.
By using this strategy, the average sleeper will increase the sleep promoting neurotransmitter adenosine in the cerebrospinal fluid to allow for natural sleep onset. This will reduce the need to add in amino acid precursors for GABA neurotransmitter or add in exogenous melatonin.
You should also bock high lux of light (intensity of light source) to below 80 lux after 6pm on a normal schedule. This is harder than it sounds, since most internal lights are well over 100 lux. Many electronics have high lux and blue wave length of light, which suppresses melatonin production. Adding a blue wave length blocking screen protector, software application or glasses may improve natural melatonin production.
Avoid electromagnetic frequencies that will disrupt slow wave sleep (SWS) generation and Rapid Eye Movement (REM) sleep. Don’t work up to the last minute. Integrate some form of relaxation to the hour before bed; less light, sleep induction mat with acupressure, heart rate variability training (NatureBeat), brain wave entrainment (Muse Headset), deep slow breathing and don’t go to bed until sleepy.
The worst thing someone with insomnia can do is to go to bed early and then lie there wide awake. One too many nights of this behavior and the unconscious brain will start associating the bed with being awake. The scary truth is that the brain will generate neurologic pathways that reflect our average sleep habits, and so 5, 10 or 20 years of ignoring our sleep needs may possibly hard wire us when we are older to be poor sleepers. This is not helpful for the average 50 year old or older person, since we tend to have less solid sleep and less deep (SWS) as we age, compounding the challenges we face with the aging brain.
The data is becoming overwhelming regarding the importance of adequate sleep time. Savvy minded folks who are looking to improve performance or simply stay at their optimal health just can’t afford to ignore sleep health. Most people need a minimum of 7 hours to 8 hours of sleep a night (not time in bed).
As you can see, the rising tide of inflammation, immune system problems, weight gain, high blood pressure and hormonal imbalances the general public is attempting to address may be avoided by tapping into our natural healing resource – sleep.
—————————————
How To Quantify Your Sleep
So how do you know you are getting adequate sleep?
The simplest answer is to monitor your vigilance during the day. If waking in the morning to an alarm clock is compulsory, or if you are falling asleep in the afternoon or during meetings or falling asleep in the evening in front of the television, you are not adequately rested. More quantified assessments of adequate sleep may include morning heart rate variability (HRV – the beat-to-beat alterations in heart rate) assessment. Blood testing showing elevated CRP may represent sleep curtailment as well. This measure would likely need to be assessed after a full week of recovery sleep, noting the long duration that CRP persists in the blood stream.
This guest post was written by Dr. Joseph Zelk, the Medical Director of the Sleep Medicine Group. In just 2 weeks, I'm releasing a podcast interview with Dr. Zelk. The interview is about a hidden sleep killer that flies under the radar, and what you can do about it. If you or a loved one struggle with sleep, you'll want to stay tuned for that audio (click here to subscribe to the free podcast in iTunes), and in the meantime, leave your questions, comments and feedback for Dr. Zelk or myself below.
Finally, for customized, cutting-edge sleep tracking and testing, a one-on-one sleep consultation via Skype, screening for obstructive sleep apnea or any other your other sleep enhancement or insomnia fixing needs, visit www.sleepmedicinegroup.com. Mention “Ben Greenfield” on your e-mail intake form or when you speak to a representative, and get a $25-100 discount on any sleep testing or sleep consulting services.














Such an important article. Thanks, Ben! Given all that we're learning about the importance of sleep, including that we can't make up for lost sleep, and the fact that poor sleep is linked to obesity and diseases that start with obesity, as well as negatively impacting brain health and aging, would you say that sleep is the #1 health habit right now? I am seriously thinking that getting adequate sleep on a consistent basis maybe should be the top priorty, followed extremely closely by good nutrition, and then NEM.
im a living proof on how real is a sleep deprivation could wreck your mind and body. I used to have a bad sleep habit since my teenage years, but it got really worse when i reach 22 that I often stayed up late and sometimes i only have 2 – 3 hours of sleep and did a heavy physical activity in the morning. This habit happened consistently for 3 years and i didnt realize that time, a poor sleep patern usually go hand on hand with a poor diet choice.
My awakening moment is when i was suddenly suffered from anxiety attack in one day after the previous night i only had 3 hours of sleep. My mind was rushing and i was really obssesive with my own thoughs. I was really afraid because i never felt that way before and though i was going crazy. I get on bed earlier that night and hoping that things would be ok for tommorow morning, but i was wrong. I keep have anxious thoughs for the next couple weeks. I experienced hot flushes, headaches, palpitations and tremors, im also depressed and feel my abilty to cope with stress is decreased, after one week i suffered that way i finally met my doctor and she was checking my Blood pressure and it was 150/100 and my cholesterol is around 229 something.
My doctor was suprised that time, because i was only 25 years old and i look like a normal healthy young lady from the outside. She asked if there is a history of hypertension in my family and i told her no. She suspected that i might have a problem with thyroid and requires me to do a check Lab. But then the results is zero, my thyroid hormones levels are all normal, she prescribed me with anti- inflamatory drugs and tell me that i should get to bed early.
After couple months, i feel my body is ok again, my blood pressure reading is 120/90 , my cholesterol drop to normal, and i finally could handle my anxiety, but it wasnt last long because again i back to my bad sleep habits. One day when i stayed up late untill 3 am, i suffered from anxiety attack again in the next day, but this one is worse because i also experienced a mild depression, when i cant enjoy any activity that i used to love, i feel hopeless and i have suicidal thoughs in my mind. I feel i cant learn anything and my brain cant process new information. This was last for weeks untill i told my self that the root of this problem is an inflamation caused by sleep deprivation.
I finally make a commitment to myself that i will keep a healthy sleep habits although it is hard for me. I also took a Fish Oil suplement and hey its only been a months and i slowly gaining my well being again, although sometimes i still have bad mood, i really gratefull that i could survive from that scary depression weeks when i feel like it was my end. Now im planning to take a melatonin suplement so i could have a better sleep, because sometimes i had a nightmares that cause me to awake.
So my messages for anyone who read this, if you love your body and soul then pleasee get a proper sleep, maintain a good sleep habits before it is too late for everything. Sleep is our basic need. I know that there are so many hypothesis out there regarding sleep but personally i believe that all living organism need a sleep or similar condition to maintain its overall being. So please have a good sleep tonight :)
Ps: Im sorry with my bad grammar since english is my third language :D